Sampling the stratum corneum is a cornerstone procedure in dermatological research and clinical diagnostics, providing a non-invasive window into the skin’s physiological state. The stratum corneum, the outermost layer of the epidermis, serves as the primary barrier against environmental insults and regulates transepidermal water loss. By collecting these superficial layers, clinicians and researchers can analyze protein expression, lipid composition, and the presence of inflammatory cytokines without the need for traditional, invasive surgical biopsies. This image illustrates a common technique used to retrieve these vital biological samples for detailed barrier analysis.
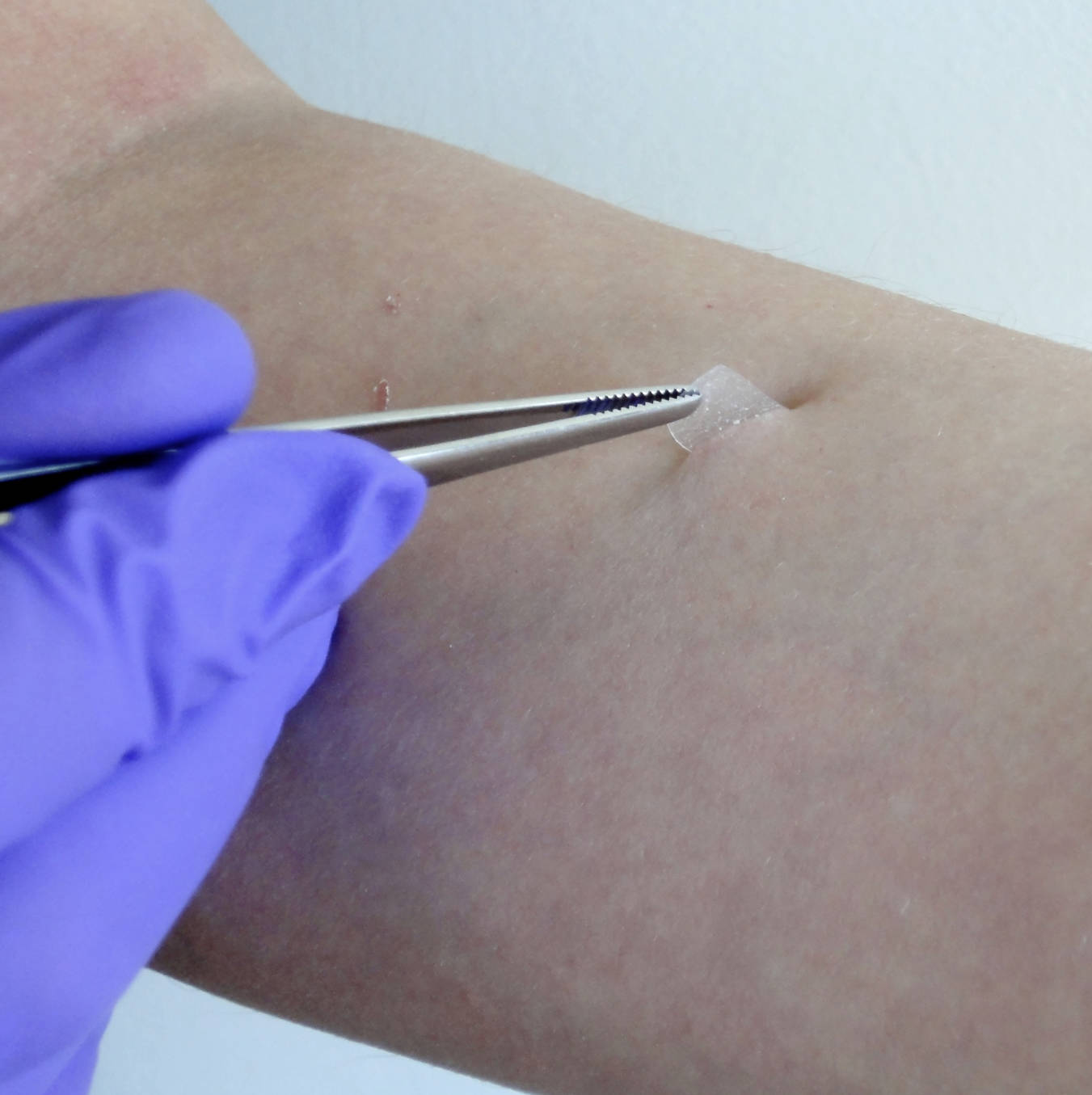
Image Overview
The image depicts a clinical or laboratory procedure involving the sampling of the human stratum corneum from the volar forearm. A healthcare professional, identified by the use of a purple nitrile glove, is utilizing fine-tipped forceps to carefully lift a small, translucent sample from the skin surface. This sample is likely a piece of specialized adhesive tape or a circular disc used in the “tape stripping” method. As the tape is pulled away, it removes several layers of corneocytes—the flattened, keratinized cells that comprise the stratum corneum—along with the interstitial lipids that surround them.
The visual evidence shows a clean, controlled environment. The skin surrounding the sampling site appears normal, though slight erythema or a “glistening” appearance may occur after multiple strips are taken, indicating the progressive removal of the protective barrier. This specific visualization highlights the delicate nature of skin sampling and the precision required to obtain high-quality biological material for subsequent analysis.
Anatomical Overview
The stratum corneum is often described using the “bricks and mortar” model. In this analogy, the corneocytes represent the bricks, and the extracellular lipid matrix (composed of ceramides, cholesterol, and free fatty acids) represents the mortar. This layer is the final product of keratinocyte differentiation, a process known as cornification. As cells move upward from the stratum basale through the stratum granulosum, they lose their nuclei and organelles, eventually becoming the tough, resilient scales seen in the image.
Sampling this layer is anatomically significant because the stratum corneum thickness varies significantly across different body regions. For instance, it is exceptionally thick on the palms and soles to withstand mechanical stress, while it is much thinner on the face or the volar forearm (the site shown in the image). The integrity of this layer is maintained by corneodesmosomes, which must be enzymatically degraded for natural desquamation to occur. Tape stripping effectively bypasses this natural shedding process to collect a concentrated snapshot of the skin’s current biochemical profile.
Clinical Relevance
In a clinical setting, sampling the stratum corneum via tape stripping has become an invaluable tool for managing and researching chronic skin conditions. In patients with atopic dermatitis, the stratum corneum often shows a deficiency in filaggrin, a key protein required for barrier function. By analyzing samples like the one in the image, clinicians can quantify cytokine levels (such as IL-4 or IL-13) to assess the severity of systemic inflammation and the effectiveness of targeted biological therapies.
Furthermore, this method is widely used in the pharmaceutical industry to evaluate the bioavailability of topical medications. Since many drugs are designed to penetrate the stratum corneum to reach the viable epidermis or dermis, measuring the concentration of the drug within the stripped layers allows researchers to create drug-penetration profiles. This ensures that topical treatments are reaching therapeutic levels without causing excessive systemic absorption or local irritation.
Diagnostic or Educational Importance
For medical learners, understanding this procedure is essential for grasping the shift toward personalized medicine and non-invasive diagnostics. Traditional punch biopsies, while definitive, carry risks of infection, scarring, and patient discomfort. Sampling the stratum corneum serves as a molecular biopsy that is virtually painless and leaves no permanent mark, making it ideal for pediatric populations or for longitudinal studies where multiple samples must be taken over time.
Educationally, the image reinforces the concept that the skin surface is not merely a “dead” layer but a metabolically active environment containing a wealth of diagnostic information. Techniques like this allow for the study of the skin microbiome, the detection of fungal pathogens, and the assessment of DNA/RNA expression within the epidermis. It bridges the gap between basic skin anatomy and advanced proteomic and transcriptomic analysis.
Summary for Medical Learners
Sampling the stratum corneum is a precise, non-invasive technique that bridges the gap between clinical observation and molecular analysis. By using adhesive strips or discs, as shown in the image, practitioners can harvest corneocytes to evaluate barrier integrity, inflammatory markers, and drug delivery efficiency. For the medical student, mastering the rationale behind this procedure is key to understanding modern dermatological research and the critical role of the epidermal barrier in systemic health. Remember that while the stratum corneum is structurally simple, its biochemical complexity is the primary defense mechanism of the human body.
Medical Learning Tips
- Always apply uniform pressure to the sampling disc or tape to ensure consistent collection of corneocyte layers across different subjects.
- Be aware that the number of tape strips required depends on the specific biomarker being analyzed and the anatomical site's thickness.
- Use fine-tipped forceps to handle the sample to prevent contamination from gloves or hands during the transfer to storage vials.

