The human skin is much more than a simple covering; it is the body’s largest organ and its first line of defense against a hostile environment. The outermost portion of the skin, known as the epidermis, is a remarkably thin but incredibly resilient structure that performs several vital roles, ranging from hydration maintenance to immunological protection. Understanding a Section of Epidermis reveals a highly organized, multi-layered epithelial tissue that is constantly renewing itself through a process called keratinization. This dynamic tissue ensures that we remain protected from ultraviolet radiation, pathogenic microorganisms, and mechanical trauma. By examining the microscopic anatomy of these layers, medical students and health professionals can gain deep insights into the pathophysiology of various dermatological conditions, such as psoriasis, eczema, and skin cancers. The complexity of the epidermis lies in its stratified squamous arrangement, where cells transform from actively dividing stem cells at the base to tough, dead protective plates at the surface.
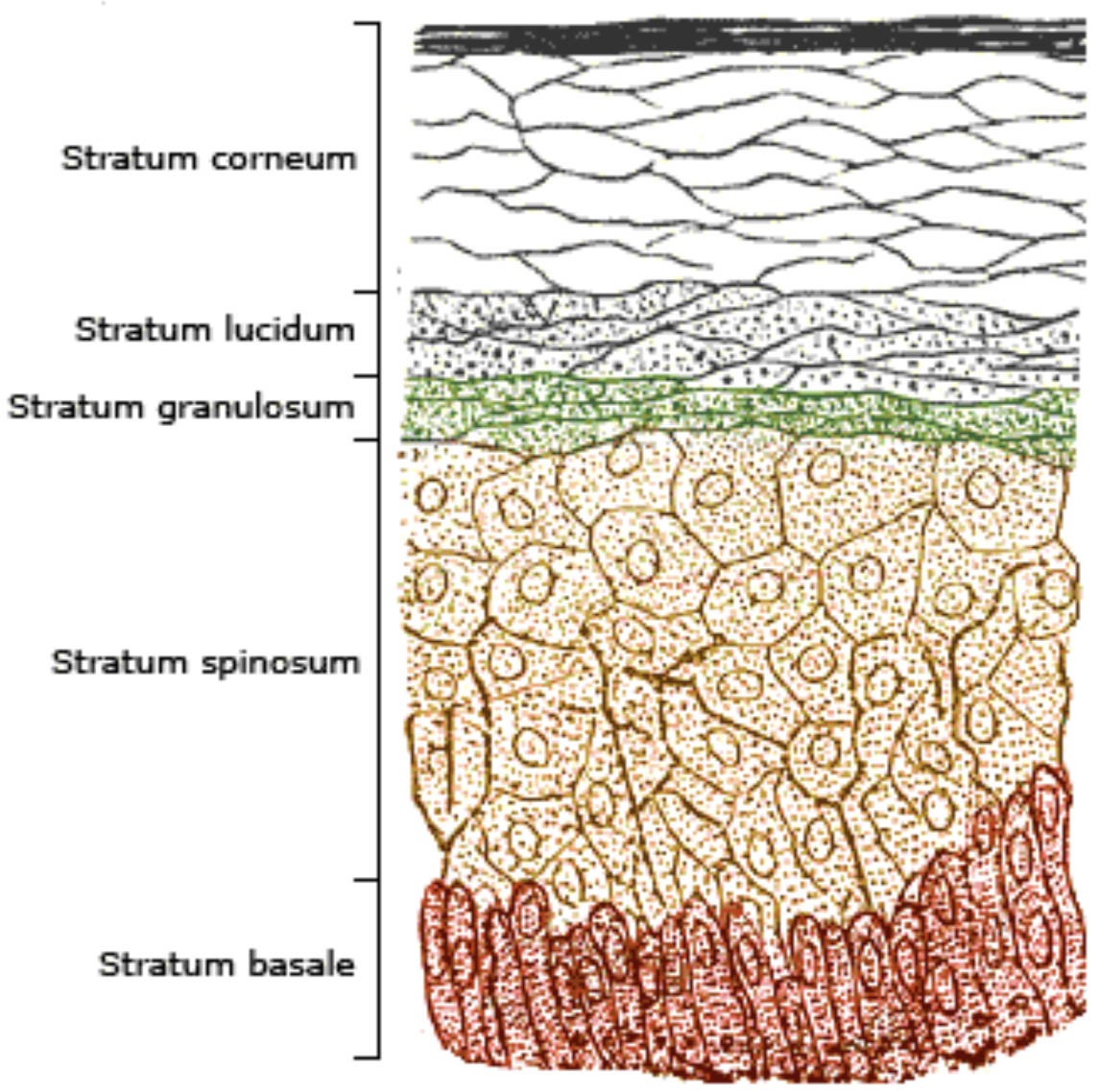
Stratum corneum: This is the most superficial layer of the epidermis, consisting of 20 to 30 layers of dead, flattened cells filled with keratin. These cells, often called corneocytes, are continuously shed and replaced from below, forming a durable waterproof barrier for the body.
Stratum lucidum: Visible only in thick skin like that of the palms and soles, this clear, thin layer consists of flattened, dead keratinocytes. It acts as an additional layer of protection to reduce friction and shear forces in areas of high mechanical stress.
Stratum granulosum: This layer marks the transition between the deeper, living metabolic layers and the superficial, dead layers of the skin. Cells here contain keratohyalin granules and begin to undergo apoptosis, flattening as their nuclei and organelles break down.
Stratum spinosum: Often called the prickly layer due to the appearance of its cells under a microscope, this thick region provides structural strength. The cells are held together by sturdy junctions that resist tension and contain Langerhans cells for immune surveillance.
Stratum basale: The deepest layer consists of a single row of stem cells that are constantly undergoing mitosis to produce new skin cells. It is also the site where the pigment-producing cells and sensory receptors are primarily located, anchoring the epidermis to the dermis.
The Dynamic Architecture of the Epidermal Layers
The epidermis is classified as a keratinized stratified squamous epithelium. Its unique structure is designed to facilitate a one-way journey for the cells that compose it. A Section of Epidermis shows that the tissue is avascular, meaning it lacks its own blood supply; instead, it relies on the diffusion of nutrients from the underlying dermis. This lack of direct blood flow is one reason why superficial scratches do not bleed, yet the tissue remains metabolically active enough to regenerate entirely every 25 to 45 days. The organization of the five strata reflects a perfect balance between cellular birth and death.
In regions of the body subjected to heavy use, such as the feet, the epidermis thickens significantly. This structural adaptation involves a more prominent stratum corneum and the inclusion of the stratum lucidum. Conversely, in delicate areas like the eyelids, the epidermis is exceptionally thin. This variability allows the skin to meet the specific mechanical and sensory needs of different body parts while maintaining a consistent defensive perimeter. The integrity of this architecture is maintained by a complex network of proteins and lipids that seal the gaps between cells.
Cellular Residents: The Role of Keratinocytes
The vast majority of cells found in any Section of Epidermis are keratinocytes. These cells are the structural workhorses of the skin, named for the tough, fibrous protein they produce. Keratin provides the skin with its characteristic durability and water-resistant properties. The lifecycle of these cells begins in the stratum basale, where they are born through mitotic division. As new cells are formed, they push older cells upward through the spinosum and granulosum layers. During this ascent, they produce increasing amounts of keratin until they eventually die and become the protective scales of the stratum corneum.
As these cells migrate, they also produce lamellar granules. These granules release a lipid-rich secretion that fills the spaces between the cells in the upper layers, effectively acting as a “mortar” between cellular “bricks.” This lipid barrier is what makes human skin nearly waterproof, preventing us from absorbing too much water when we swim and, more importantly, preventing our internal fluids from evaporating into the air. Without the continuous production and maturation of these cells, the body would quickly succumb to dehydration and infection.
Pigmentation and Protection: The Influence of Melanocytes
While the structural frame is built by other cells, the color and UV-protective qualities of the skin are determined by melanocytes. These spider-shaped cells are primarily found in the stratum basale. They produce a pigment called melanin, which is packaged into granules known as melanosomes. These granules are then transferred to the neighboring cells, where they gather on the sunny side of the cell nucleus. This clever biological mechanism acts like a tiny parasol, shielding the precious DNA from the damaging effects of ultraviolet (UV) radiation.
The number of these pigment-producing cells is actually quite similar across different human ethnicities; the variation in skin color arises from the type of pigment produced and how long the granules persist in the upper layers of the skin. When we are exposed to sunlight, these cells increase their production of pigment, resulting in a tan. This is an adaptive response designed to prevent mutations that could lead to skin cancer. However, this protection is not absolute, and overexposure to UV light can still damage the deeper layers of the Section of Epidermis, highlighting the importance of external sun protection.
Mechanical Strength and Cellular Adhesion
The ability of the skin to stretch and resist tearing is largely due to the specialized connections between its cells. In the stratum spinosum, the cells are tightly bound together by desmosomes. These are protein complexes that act like rivets, tethering the intermediate filaments of one cell to those of its neighbor. Under a microscope, when the cells shrink during preparation, these connections pull on the cell membranes, creating the “spiny” appearance that gives the layer its name. These junctions are crucial for maintaining the mechanical integrity of the epidermis under stress.
Beyond mechanical strength, these connections allow the epidermis to act as a unified sheet rather than a collection of loose cells. This is particularly important in the stratum granulosum, where the cells begin to flatten and die. The desmosomes ensure that even as the cells lose their internal vitality, they remain locked together to form a cohesive barrier. If these connections are disrupted by genetic disorders or autoimmune diseases, the skin may blister or peel away with even the slightest touch, demonstrating how essential cellular adhesion is to our daily survival.
Clinical Significance of Epidermal Histology
Understanding the Section of Epidermis is fundamental to clinical dermatology. Many skin diseases are essentially disruptions of the normal epidermal lifecycle or structure. For instance, psoriasis is a condition where the turnover of cells is drastically accelerated. Instead of taking a month to migrate from the base to the surface, cells reach the top in just a few days. Because they have not had time to mature or shed properly, they pile up into thick, silvery scales that are both itchy and painful. Treating such conditions often involves slowing down the rate of cell division or normalizing the maturation process.
- Basal Cell Carcinoma: The most common form of skin cancer, arising from the stem cells in the stratum basale. It is typically slow-growing and rarely spreads but can be locally invasive.
- Squamous Cell Carcinoma: Arises from the keratinocytes in the stratum spinosum. It tends to grow more rapidly than basal cell carcinoma and has a higher potential to metastasize if not treated early.
- Melanoma: The most dangerous form of skin cancer, originating in the melanocytes. Because these cells are highly mobile, this cancer can spread quickly to other parts of the body.
- Eczema and Dermatitis: Often involve a breakdown in the lipid barrier of the stratum corneum, allowing irritants and allergens to penetrate the living layers and trigger inflammation.
The Sensory and Immunological Functions
Though the epidermis is primarily protective, it is also an active sensory and immunological organ. Scattered throughout the stratum basale are Merkel cells, which are associated with sensory nerve endings. These cells allow us to perceive the sensation of light touch, making the skin a primary tool for interacting with our environment. Additionally, the stratum spinosum contains Langerhans cells (epidermal dendritic cells). These cells are part of the immune system; they act as sentinels that capture foreign invaders and transport them to the nearest lymph node to trigger an immune response.
This dual functionality ensures that the skin is not just a wall, but a “smart” barrier. It can sense the environment, respond to injury, and call for help from the rest of the body when needed. The integration of nervous, immune, and epithelial systems within such a thin Section of Epidermis is a testament to the efficiency of human evolution. Whether it is healing a minor cut or mounting a defense against a viral infection, the layers of the epidermis work in perfect concert to maintain the body’s internal homeostasis.
Conclusion: The Essential Barrier of Life
In conclusion, the epidermis is a masterpiece of biological engineering. From the rapid cellular birth in the stratum basale to the tough, protective shield of the stratum corneum, every layer has a specific and necessary function. The Section of Epidermis highlights a journey of transformation that every skin cell must take to keep the organism safe and hydrated. By respecting the roles of keratinocytes and melanocytes, and understanding the strength provided by desmosomes, we can better care for our skin and recognize the early signs of disease. The skin is far more than a cosmetic feature; it is a vital, living organ that demands our attention and protection. As the interface between our inner selves and the outer world, the epidermis remains one of the most important components of human health and survival.
Section of Epidermis, Stratum corneum, Stratum basale, Skin Histology, Dermatology, Keratinization, Integumentary System, Melanocytes, Keratinocytes, Skin Barrier

