The cardiovascular system is a marvel of biological engineering, relying on a network of vessels that must be both incredibly strong and remarkably flexible. To appreciate how our bodies manage blood pressure and nutrient delivery, one must look beyond the macroscopic view and investigate the Microscopic Anatomy of an Artery. Every artery in the body is more than just a hollow tube; it is a complex, living organ composed of specialized cells and extracellular matrices organized into distinct functional layers. These microscopic components work in harmony to sense changes in blood chemistry, respond to physical stress, and maintain the integrity of the circulatory system. By understanding the cellular and histological features of the arterial wall, medical students and professionals can better comprehend the mechanisms of vascular health and the origins of systemic diseases. This article explores the intricate details of the arterial wall, from the delicate endothelial lining to the robust connective tissues that provide structural support.
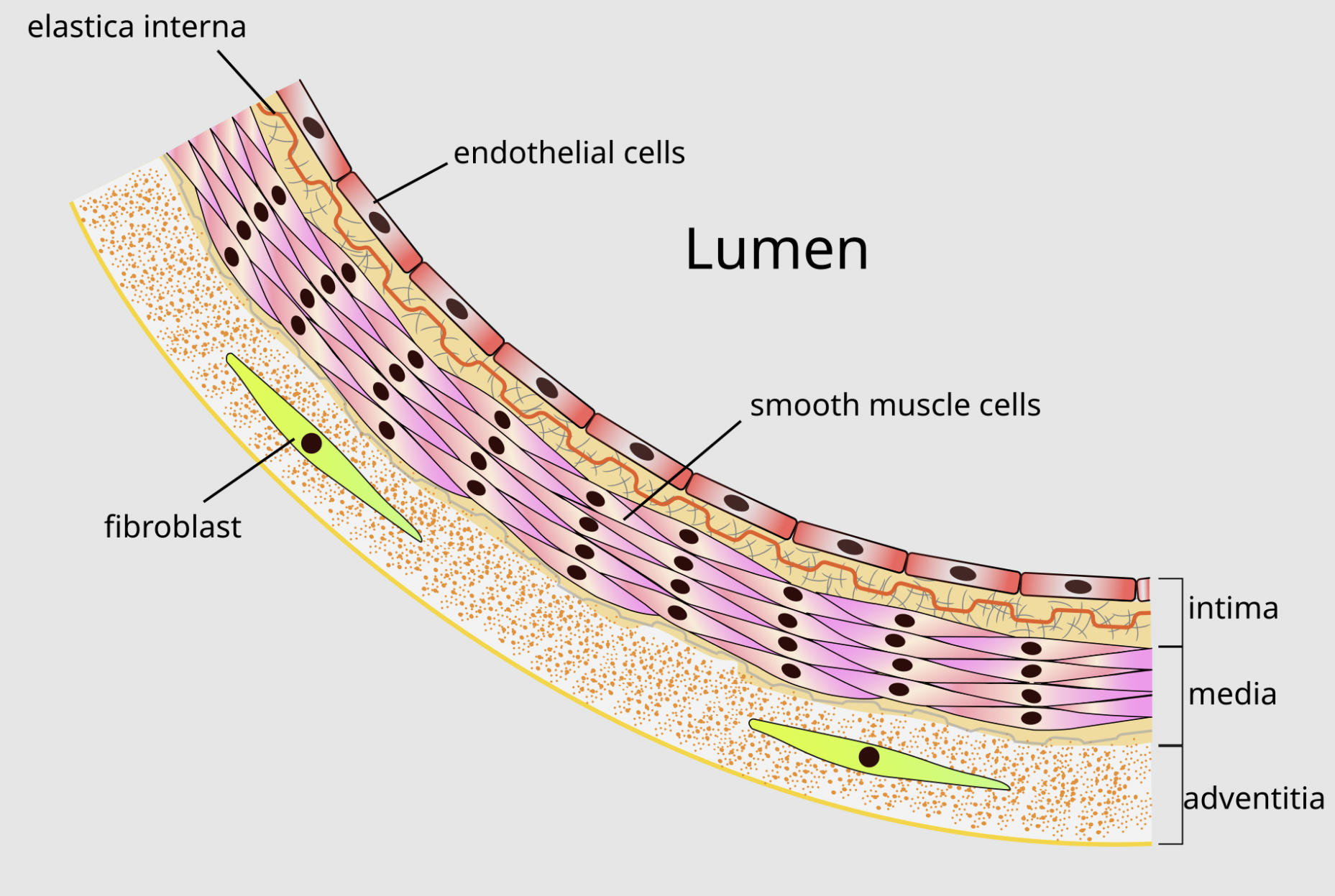
elastica interna: This layer consists of a dense network of elastic fibers that form a wavy boundary between the tunica intima and the tunica media. It allows the artery to expand significantly during the heart’s contraction and recoil during the resting phase to maintain continuous blood flow.
endothelial cells: These are thin, squamous cells that form a continuous, smooth surface lining the entire vascular system to minimize friction. They play a crucial role in vascular homeostasis by releasing signaling molecules that regulate blood clotting and the relaxation of the vessel wall.
Lumen: This is the central hollow space of the blood vessel through which blood is transported throughout the body. The width of this space is dynamic and is constantly adjusted by the surrounding muscular layers to meet the metabolic demands of different tissues.
smooth muscle cells: Located primarily in the tunica media, these spindle-shaped cells are responsible for the contraction and relaxation of the vessel. By changing their tension, these cells control the diameter of the lumen and, consequently, the resistance to blood flow and systemic blood pressure.
fibroblast: These cells reside in the outermost layer of the artery and are responsible for secreting collagen and other components of the extracellular matrix. They provide the necessary scaffolding and structural integrity to prevent the artery from over-expanding or rupturing under pressure.
intima: The tunica intima is the innermost layer of the arterial wall, encompassing the endothelium and a thin layer of connective tissue. It serves as the primary interface between the circulating blood and the vessel wall, acting as a selective barrier for nutrients and waste.
media: This is the middle and typically the thickest layer of the artery, composed of layers of smooth muscle and elastic tissue. It provides the mechanical strength required to withstand the high pressure of oxygenated blood pumped directly from the heart.
adventitia: Also known as the tunica externa, this is the protective outer layer composed of loose connective tissue, nerves, and small blood vessels. It anchors the artery to surrounding tissues and provides the vessel with its own dedicated nutrient supply through the vasa vasorum.
The Cellular Microenvironment of the Tunica Intima
At the microscopic level, the tunica intima is far more than a simple liner. It is a highly active biological interface. The endothelial cells that make up the innermost portion of the intima are incredibly sensitive to their environment. They can detect shear stress—the physical force of blood flowing over their surface—and respond by producing chemical messengers like nitric oxide. This signaling is essential for maintaining vascular health, as it tells the underlying muscle layers when to relax and ensures that blood platelets do not stick to the vessel wall, which could lead to dangerous clots.
Beneath the endothelium lies the subendothelial layer, a thin region of loose connective tissue. This area is particularly significant in clinical medicine because it is the site where atherosclerosis often begins. When the endothelial barrier is damaged by high blood pressure, toxins, or elevated glucose levels, fats and inflammatory cells can infiltrate this space. Over time, these materials accumulate, leading to the thickening of the intima and the narrowing of the lumen, which can eventually restrict blood flow to vital organs.
Mechanical Resilience: The Role of Smooth Muscle and Elastica
The tunica media is the mechanical powerhouse of the artery. It is dominated by smooth muscle cells that are arranged in a circular or spiral fashion around the lumen. This orientation is anatomically perfect for controlling the diameter of the vessel. Unlike skeletal muscle, smooth muscle can maintain a state of contraction, known as vascular tone, for long periods without fatiguing. This persistent tone is what allows the body to maintain a baseline blood pressure and quickly redirect blood to areas in need, such as the muscles during exercise or the digestive tract after a meal.
Interspersed within the muscle layers are elastic fibers, which are most concentrated in the elastica interna and elastica externa. These membranes act like biological rubber bands. When the heart pumps a surge of blood into the arteries (systole), these elastic layers stretch, absorbing the energy and preventing the pressure from rising too high. Between heartbeats (diastole), the elastic recoil of these fibers pushes the blood forward. This microscopic feature ensures that blood flow is relatively smooth and continuous, rather than a series of violent, jerky pulses that could damage delicate capillaries.
Structural Integrity and the Adventitial Fibroblasts
The tunica adventitia provides the final layer of defense and support for the arterial wall. While it may appear less active than the inner layers, its role is critical for the overall stability of the vessel. The primary cell type here is the fibroblast. Fibroblasts are the “architects” of the connective tissue, constantly producing collagen fibers that give the artery its tensile strength. This collagen prevents the artery from over-distending; it essentially sets the limit for how much the vessel can expand, acting as a safety net during sudden spikes in blood pressure.
Furthermore, the adventitia contains its own micro-circulatory system known as the vasa vasorum. Because the walls of large arteries are so thick, oxygen and nutrients from the blood in the lumen cannot diffuse all the way to the outer layers. The vasa vasorum consists of tiny capillaries that penetrate the adventitia to nourish the living cells of the outer wall. Similarly, the nervi vasorum—a network of autonomic nerves—travels through the adventitia to reach the smooth muscle of the media, allowing the brain to control the vessel’s diameter instantaneously.
Clinical Implications: Microscopic Changes in Vascular Disease
Many of the most common cardiovascular diseases are fundamentally disorders of the microscopic anatomy. In chronic hypertension, for example, the constant high pressure forces the tunica media to undergo hypertrophy. The smooth muscle cells increase in size and number to handle the load, but this makes the vessel wall stiffer and the lumen narrower, creating a dangerous cycle of increasing resistance. Similarly, aging leads to the gradual degradation of the elastica interna, resulting in “hardening of the arteries” and a loss of the pressure-buffering capacity of the vessel.
- Endothelial Dysfunction: The loss of the endothelium’s ability to produce nitric oxide, leading to chronic vasoconstriction and increased risk of clotting.
- Medial Calcification: The deposition of calcium within the tunica media, which often occurs in patients with kidney disease or diabetes, further reducing vessel flexibility.
- Aneurysm Formation: A localized weakening of the media and adventitia that allows the wall to bulge outward, often due to the degradation of collagen and elastic fibers.
- Plaque Rupture: The microscopic breakdown of the fibrous cap covering an atherosclerotic lesion, which exposes the blood to highly thrombogenic materials within the wall.
Maintaining the Microscopic Health of Arteries
Preserving the Microscopic Anatomy of an Artery is the cornerstone of longevity and heart health. Lifestyle choices have a direct impact on the cellular health of these vessels. Antioxidant-rich diets protect the endothelial cells from oxidative stress, while regular cardiovascular exercise promotes the elasticity of the media and the efficiency of the vasa vasorum. Furthermore, managing blood glucose and cholesterol levels prevents the infiltration of harmful substances into the subendothelial space, keeping the tunica intima thin and smooth.
In the modern medical era, we also have pharmacological tools designed to target these microscopic layers. Statins not only lower cholesterol but also have “pleiotropic” effects that stabilize the endothelium and reduce inflammation within the adventitia. Blood pressure medications like ACE inhibitors help protect the smooth muscle cells from the damaging effects of chronic overwork. By treating the artery at the microscopic level, we can prevent the macroscopic failures—such as heart attacks and strokes—that are the leading causes of mortality worldwide.
Conclusion: A Symbiotic System of Layers
The microscopic structure of the artery is a testament to the complexity of human life. Each layer—the intima, media, and adventitia—performs a unique and indispensable role, ranging from biochemical signaling and mechanical force to structural anchoring. The Microscopic Anatomy of an Artery illustrates how specialized cells like fibroblasts and endothelial cells coordinate their efforts to ensure the survival of the organism. Understanding these tiny details provides the foundation for all of vascular medicine, reminding us that the health of the entire body begins with the integrity of its smallest cellular components. By respecting and protecting these intricate layers, we can maintain the resilience of the circulatory system for decades to come.

