The cardiovascular system is often celebrated for the powerful delivery of oxygenated blood through the high-pressure arterial network, but the unsung hero of systemic circulation is the venous system. Tasked with the monumental challenge of returning deoxygenated blood against the persistent force of gravity, veins utilize a unique anatomical design to ensure efficient flow back to the heart. Unlike arteries, which must endure explosive pressure surges from cardiac contractions, the Vein Wall is thinner and significantly more flexible, allowing it to act as a dynamic reservoir for the body’s blood volume. This educational guide explores the microscopic layers that constitute the venous structure, the functional importance of one-way valves, and the physiological adaptations that prevent the pooling of blood in the lower extremities. By understanding the histopathology and mechanical properties of these vessels, we can better appreciate how the body maintains circulatory balance under varying physiological conditions.
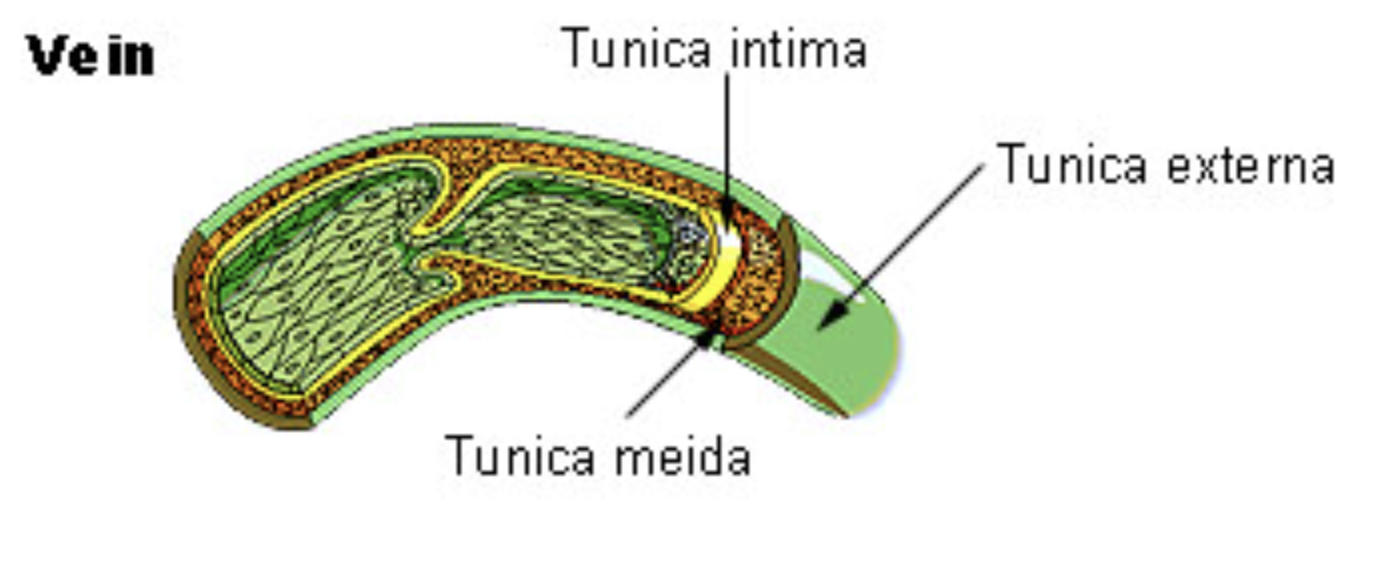
Tunica intima: This is the innermost layer of the vein wall, consisting of a smooth endothelial lining and a thin subendothelial layer of connective tissue. It provides a frictionless surface for blood cells and often extends into the lumen to form the structural basis of venous valves.
Tunica meida: Labeled in the diagram as the middle layer, this section is composed of smooth muscle and elastic fibers, though it is significantly thinner than its counterpart in arterial walls. Its primary function is to provide the vessel with the tone necessary to move blood forward without having to resist extreme pressures.
Tunica externa: This is the outermost layer of the vein, made up of heavy collagenous fibers that offer structural support and prevent the vessel from over-expanding. In the largest veins, this layer can be the thickest part of the wall, sometimes containing longitudinal bundles of smooth muscle to help facilitate the return of blood.
The Architecture of the Vein Wall
The histological makeup of the venous system follows a general three-layered pattern, yet it is modified to suit low-pressure environments. The tunica intima is the most delicate layer, featuring a single layer of squamous endothelial cells. These cells are not merely a passive barrier; they are metabolically active, releasing factors that regulate blood clotting and local vessel tone. In veins, the internal elastic lamina—a prominent feature in arteries—is either extremely thin or entirely absent, reflecting the lower mechanical stress placed upon the vessel lining.
Moving outward, the tunica media (often misspelled as “meida” in older diagrams) is the muscular engine of the vessel. In veins, this layer contains relatively few layers of smooth muscle and a sparse distribution of elastic fibers. This thinness is a functional adaptation. Because veins do not experience the pulse pressure of the heart, they do not require the thick muscular reinforcement seen in arteries. This lack of muscle mass makes veins highly distensible, meaning they can stretch to hold a large volume of blood with very little increase in internal pressure. Finally, the tunica externa (or adventitia) provides the necessary scaffolding. In large veins like the vena cava, the tunica externa is robust and contains vasa vasorum—tiny blood vessels that supply the thick wall itself—ensuring that even the outermost tissues remain oxygenated.
Capacitance and Compliance: Veins as Blood Reservoirs
One of the most critical physiological concepts regarding venous anatomy is that they are considered capacitance vessels. In a resting human, approximately 60% to 70% of the total blood volume is contained within the venous system at any given time. This capacity to hold blood is a direct result of the thin, compliant nature of the venous wall. Because the walls are less rigid than those of arteries, they can expand easily to accommodate fluctuations in blood volume.
This reservoir function is vital during periods of physical exertion or injury. When the body detects a drop in blood pressure or an increased demand for oxygen, the sympathetic nervous system triggers the smooth muscle in the tunica media to contract. This process, known as venoconstriction, reduces the volume of the venous reservoir and shifts blood into the arterial side of the circulation. This “auto-transfusion” mechanism helps maintain cardiac output and blood pressure during hemorrhage or intense exercise, showcasing the active role veins play in hemodynamic stability.
The Vital Role of Venous Valves
Because the pressure in veins is so low—often dropping to nearly zero near the right atrium of the heart—gravity poses a significant obstacle to blood return from the legs and feet. To overcome this, the tunica intima of many veins folds inward to create venous valves. These are bicuspid, flap-like structures that function as one-way gates. They allow blood to flow toward the heart but close shut to prevent backflow (reflux) when gravity or pressure attempts to pull blood downward.
Valves are most numerous in the veins of the lower extremities, where the vertical distance to the heart is greatest. The efficiency of these valves is dependent on the integrity of the surrounding vessel wall. If the vein wall becomes excessively stretched or weakened, the valve leaflets may no longer meet in the center, leading to a condition where blood pools in the vessel. This mechanical failure is a primary contributor to vascular pathologies and highlights why the structural health of the tunica layers is essential for systemic health.
Hemodynamic Challenges and the Skeletal Muscle Pump
The return of blood through the veins is not solely dependent on the heart’s residual pressure; it requires external assistance. The primary mechanism for this is the skeletal muscle pump. As we walk or move, the large muscles in our calves and thighs contract, squeezing the deep veins situated between them. Because of the one-way valves, this squeezing action forces blood upward toward the heart. When the muscle relaxes, the valves below the muscle close to prevent backflow, and the vein refills from the superficial system.
In addition to the skeletal muscle pump, the respiratory pump assists venous return. During inhalation, the diaphragm moves downward, increasing pressure in the abdominal cavity and decreasing pressure in the thoracic cavity. This pressure gradient effectively “sucks” blood from the abdominal veins into the thoracic veins and into the heart. These mechanisms demonstrate that the venous system is an integrated part of the body’s kinetic movement, relying on both internal anatomy and external physical activity to function optimally.
Common Pathologies of the Venous System
When the structural integrity of the vein wall is compromised, several clinical conditions can arise. One of the most common is the development of varicose veins. This occurs when the walls of superficial veins lose their elasticity and become permanently dilated. As the vessel widens, the valves become incompetent, leading to chronic blood pooling, swelling, and discomfort. This is often seen in individuals who stand for long periods, as the constant hydrostatic pressure eventually fatigues the tunica layers.
A more serious condition is Deep Vein Thrombosis (DVT), which involves the formation of a blood clot within a deep vein, usually in the leg. DVT is particularly dangerous because the clot can break loose and travel to the lungs, causing a pulmonary embolism. The risk of DVT is increased by stasis (slow blood flow), which can occur during long flights or periods of immobilization. Proper venous health involves maintaining the strength of the vessel walls and ensuring that the “pumping” mechanisms of the body are frequently engaged through movement and hydration.
Conclusion: Integrating Form and Function
The study of the vein wall reveals a masterpiece of biological engineering tailored for efficiency and resilience. While it may lack the muscular bulk of an artery, its thin, layered structure allows for the flexibility and storage capacity required to manage the body’s total blood volume. From the smooth endothelium that facilitates flow to the collagen-rich externa that provides strength, every component is vital for the safe return of blood to the heart. Understanding these structures not only aids in the diagnosis of vascular diseases but also reinforces the importance of physical activity in supporting our internal transport systems. As we continue to explore the complexities of human anatomy, the venous system stands as a testament to the body’s ability to adapt its architecture to meet the unique challenges of low-pressure fluid dynamics.

