In the high-stakes world of neurology and vascular surgery, the ability to visualize the intricate network of arteries supplying the brain without invasive intervention is a cornerstone of modern diagnostics. Magnetic Resonance Angiography (MRA) stands as a pinnacle of this capability, utilizing the powerful physics of nuclear magnetic resonance to create detailed maps of blood flow. Unlike traditional angiography, which requires catheters and ionizing radiation, MRA offers a safer, yet remarkably clear, perspective on the arterial structures from the heart to the brain. This technology does more than just show where the blood is; it provides insights into the speed, direction, and turbulence of flow, allowing clinicians to detect life-threatening conditions like aneurysms or severe stenosis before they manifest as a stroke. As we delve into the anatomical landscape revealed by an MRA, we appreciate the complex engineering of the human body and the sophisticated tools we use to protect its most vital organ.
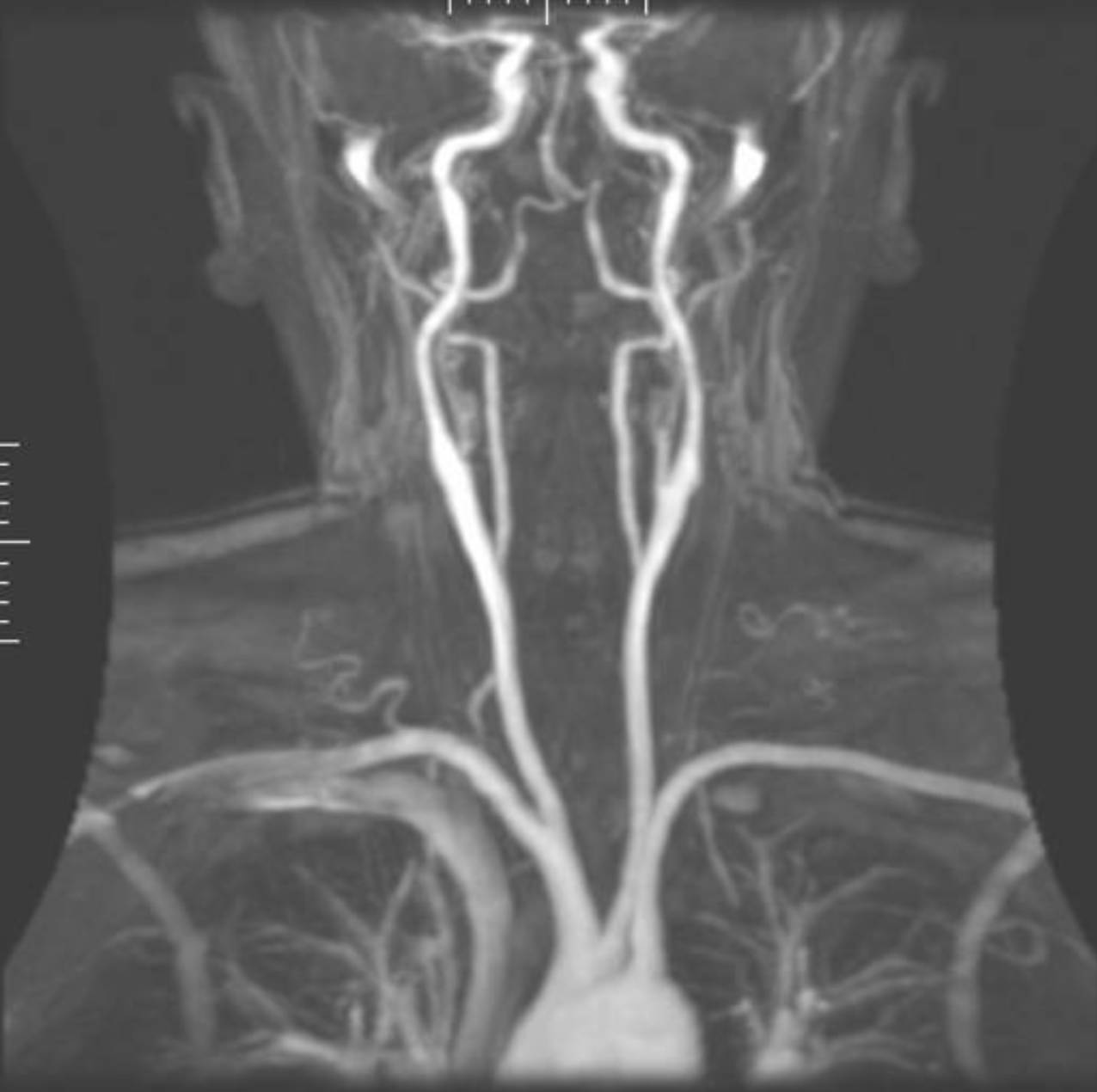
Aortic Arch: This is the large, luminous structure at the base of the image, serving as the central distribution hub from which all major arteries to the head, neck, and arms originate. Its healthy curvature and smooth lumen are essential for maintaining the high-pressure flow required to reach the cerebral circulation.
Common Carotid Arteries: These are the two thick, vertical vessels ascending on either side of the trachea, acting as the primary conduits for oxygenated blood. Their clarity in this scan is vital for identifying any atherosclerotic plaque buildup that could lead to carotid artery disease.
Subclavian Arteries: These vessels branch horizontally away from the midline towards the shoulders, supplying blood to the arms. They also give rise to the vertebral arteries, making them a critical junction in the systemic and cerebral vascular networks.
Vertebral Arteries: These thinner vessels are seen running parallel to the carotids but positioned more posteriorly, travelling through the cervical vertebrae. They converge within the skull to form the basilar artery, which provides blood to the brainstem and posterior brain regions.
Carotid Bifurcation: This is the Y-shaped split in the upper neck where the common carotid divides into internal and external branches. This area is a common site for turbulence and the formation of plaque, making it a focal point for diagnostic monitoring.
Internal Carotid Arteries: These vessels are the direct continuation of the common carotid into the cranial cavity, providing the majority of the blood supply to the cerebral hemispheres. In the MRA, their tortuous path as they enter the skull is clearly visualized, showing the natural adaptation to maintain steady pressure.
The Technological Foundation of MRA
Magnetic Resonance Angiography operates on two primary modalities: Time-of-flight (TOF) and contrast-enhanced MRA. TOF imaging is particularly fascinating because it requires no injections; it relies solely on the movement of protons within the blood. As blood flows into a thin “slice” of the magnet’s field, it produces a signal that differentiates it from the stationary surrounding tissue. This allows for a completely non-invasive visualization of the arterial tree, which is ideal for routine screening or for patients with renal failure who cannot tolerate contrast agents.
In contrast-enhanced MRA, a paramagnetic substance, usually Gadolinium, is injected into the venous system. This agent significantly shortens the relaxation time of blood, making the vessels appear extremely bright and sharp. Contrast enhancement is often preferred when looking at the large vessels of the chest and neck, such as the aortic arch, because it provides a much faster scan time and is less sensitive to patient movement. Both methods culminate in a 3D reconstruction known as a Maximum Intensity Projection (MIP), which is the specific type of image shown above, allowing the radiologist to rotate the vascular tree and examine it from every possible angle.
Visualizing the Great Vessels: Aortic Arch to Neck
The journey of blood to the brain begins at the aortic arch. In the MRA image, we can see the three primary branches originating from the top of the arch: the brachiocephalic trunk (which further divides into the right subclavian and right common carotid), the left common carotid artery, and the left subclavian artery. This anatomical arrangement is known as the “normal” branching pattern, though MRA is excellent at detecting variations, such as the “bovine arch,” which occurs in about 15% of the population. Mapping these vessels is the first step in understanding a patient’s risk for systemic vascular disease.
As the vessels ascend into the neck, the focus shifts to the carotids and vertebrals. The carotid arteries provide the anterior circulation, while the vertebral arteries provide the posterior circulation. These two systems are designed with redundancy in mind, eventually meeting inside the skull to form the Circle of Willis. MRA is uniquely suited to visualize this redundancy, allowing doctors to see how well one system can compensate if another becomes narrowed or blocked. This “collateral flow” is often the difference between a minor incident and a debilitating stroke.
Clinical Utility in Stroke and Vascular Disease
One of the most common reasons for ordering a neck MRA is to evaluate the degree of carotid stenosis. Over time, lipids and calcium can build up in the arterial walls, a process known as atherosclerosis. The carotid bifurcation is especially prone to this because of the natural turbulence created at the split. An MRA can accurately measure the percentage of narrowing in the vessel lumen, helping surgeons decide if a procedure like an endarterectomy or stenting is necessary to restore flow and prevent future neurological events.
Beyond simple narrowing, MRA is the gold standard for detecting arterial dissections and aneurysms. A dissection occurs when a tear in the inner layer of the artery allows blood to enter the wall of the vessel, creating a “false lumen.” This is a common cause of stroke in young adults and can be triggered by trauma or even sudden neck movements. Because MRA can distinguish between the layers of the vessel wall and the blood within them, it is exceptionally sensitive for catching these dangerous injuries early in their progression.
Comparative Advantages in Radiological Imaging
When clinicians choose between MRA, CTA (Computed Tomography Angiography), and conventional catheter-based angiography, they weigh several factors. CTA is incredibly fast and offers superior visualization of calcified plaques, but it requires a significant dose of ionizing radiation and iodine-based contrast, which can be hard on the kidneys. Conventional angiography remains the “gold standard” for detail and allows for immediate treatment (like placing a stent), but it is an invasive surgery with risks of bleeding and stroke.
- Safety: MRA is the safest option for long-term monitoring as it uses no radiation.
- Soft Tissue Contrast: MRA provides better visualization of the vessel wall itself, not just the hollow lumen.
- Versatility: MRA can assess flow velocity and volume, adding a functional layer to the anatomical data.
- Accessibility: While more expensive and time-consuming than CT, MRA is becoming the preferred first-line tool for elective vascular workups.
Patient Considerations and Safety Protocols
Despite its many benefits, MRA is not suitable for everyone. Because it uses an incredibly powerful magnetic field, patients with certain metal implants, such as older pacemakers, cochlear implants, or certain types of aneurysm clips, cannot enter the machine. Modern implants are increasingly “MR-safe,” but a rigorous screening process is mandatory before every scan. Furthermore, patients with claustrophobia may find the narrow, loud tunnel of the MRI scanner challenging, though many modern facilities now offer “open” magnets or sedation to assist these individuals.
The scan itself typically takes between 30 and 60 minutes. During this time, the patient must remain perfectly still, as even small movements can cause “motion artifacts” that blur the fine details of the smaller arteries like the vertebrals. For many patients, the peace of mind provided by a clear MRA is well worth the time spent. By providing a clear, high-resolution view of the cerebrovascular highway, MRA empowers both physicians and patients to take proactive steps in managing cardiovascular health and preventing the onset of chronic disease.
Conclusion
Magnetic Resonance Angiography is a testament to the power of modern medical imaging. By transforming invisible magnetic signals into a vivid map of the body’s life-sustaining arteries, it has revolutionized how we diagnose and treat vascular disorders. From the majestic curve of the aortic arch to the delicate split of the carotid bifurcation, MRA provides the clarity and detail necessary to navigate the complexities of human anatomy. As technology continues to advance, we can expect MRA to become even faster and more detailed, further solidifying its role as an indispensable tool in the fight against stroke and cardiovascular disease. Protecting our circulation is a lifelong journey, and MRA is the map that helps us find the way.

