The parathyroid glands, small but essential endocrine organs, are embedded in the posterior surface of the thyroid gland, playing a critical role in calcium regulation. This article examines their anatomical placement and microscopic composition, offering insights into their structure and function through detailed posterior and tissue-level views.
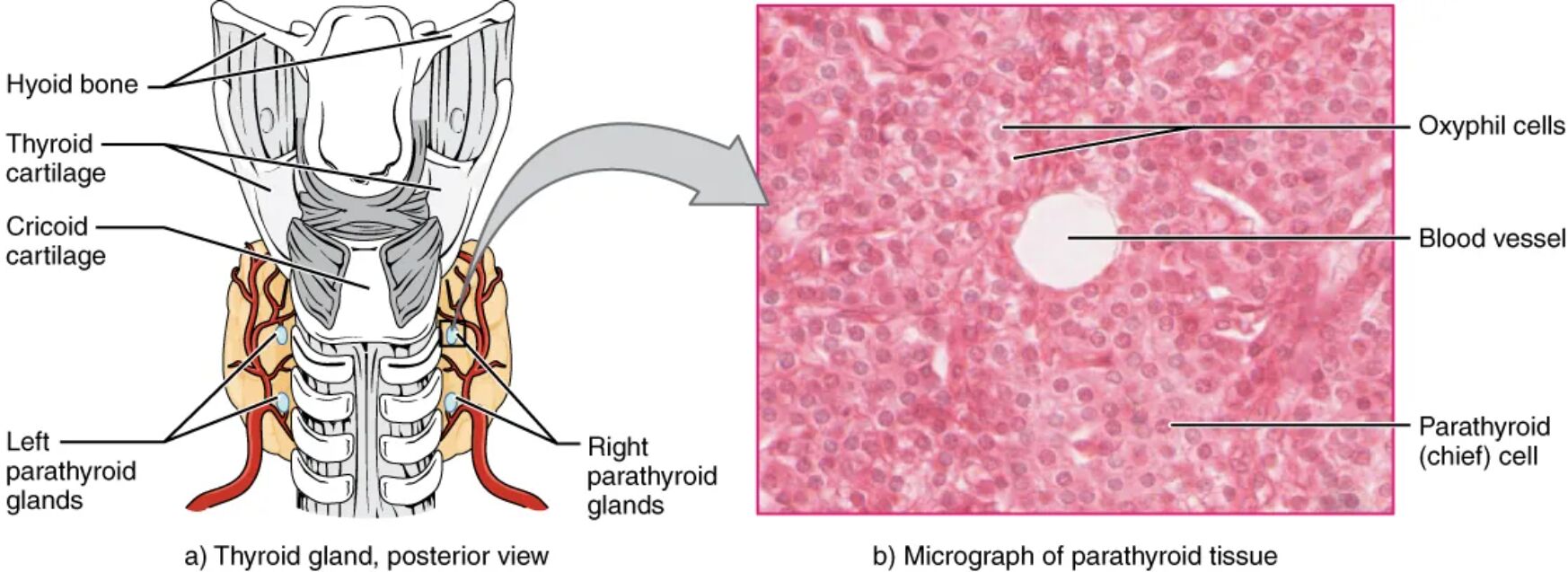
Hyoid bone The hyoid bone is located above the thyroid gland, providing structural support to the neck. It serves as an anchor for the tongue and larynx, indirectly stabilizing the parathyroid glands’ position.
Thyroid cartilage The thyroid cartilage, or Adam’s apple, protects the larynx and supports vocal cords. It frames the upper region where the parathyroid glands are situated on the thyroid’s posterior side.
Cricoid cartilage The cricoid cartilage forms the base of the larynx, sitting below the thyroid cartilage. It offers additional support to the lower thyroid and parathyroid region.
Left parathyroid glands The left parathyroid glands are embedded on the thyroid’s left posterior surface, secreting parathyroid hormone (PTH) to regulate blood calcium. Their small size belies their importance in maintaining mineral homeostasis.
Right parathyroid glands The right parathyroid glands mirror the left, located on the thyroid’s right posterior side, releasing PTH to control calcium levels. Their bilateral placement ensures balanced endocrine function.
Oxyphil cells Oxyphil cells are larger, acidophilic cells found in parathyroid tissue, increasing in number with age. Their exact role remains unclear, but they may support calcium regulation under certain conditions.
Blood vessel The blood vessel within parathyroid tissue delivers oxygen and nutrients to the cells. It facilitates the transport of PTH into the bloodstream for systemic effects.
Parathyroid (chief) cell Parathyroid (chief) cells are the primary hormone-producing cells, secreting PTH to raise blood calcium levels. These cells are most abundant and active in maintaining calcium balance.
Anatomical Overview of the Parathyroid Glands
The parathyroid glands’ location on the thyroid’s posterior surface is key to their function. This positioning allows close interaction with the thyroid while maintaining distinct roles.
- The hyoid bone and thyroid cartilage provide upper structural support to the neck region.
- The cricoid cartilage stabilizes the lower thyroid, indirectly aiding parathyroid placement.
- The left and right parathyroid glands are typically four in number, embedded in thyroid tissue.
- Their posterior location ensures efficient blood supply and hormone distribution.
- The glands’ small size makes them challenging to identify without magnification.
Microscopic Structure of Parathyroid Tissue
The micrograph reveals the cellular makeup of the parathyroid glands at 760x magnification. This view highlights the specialized cells within the tissue.
- Oxyphil cells appear larger and more eosinophilic, possibly aiding in reserve function.
- Blood vessels ensure nutrient delivery and hormone transport to the bloodstream.
- Parathyroid (chief) cells dominate the tissue, actively producing PTH.
- The dense cellular arrangement supports rapid hormonal response to calcium changes.
- The micrograph, courtesy of the University of Michigan, offers a detailed cellular perspective.
Physiological Role of the Parathyroid Glands
The parathyroid glands regulate blood calcium through PTH secretion. This function is vital for bone health, muscle function, and nerve signaling.
- PTH increases blood calcium by stimulating bone resorption and kidney reabsorption.
- Chief cells adjust PTH release based on calcium sensor feedback.
- Oxyphil cells may play a supportive role, though their function is less defined.
- Blood vessels facilitate rapid PTH distribution to target organs.
- This regulation prevents hypocalcemia and supports overall metabolic stability.
Clinical Relevance and Diagnostic Considerations
Understanding parathyroid anatomy aids in diagnosing calcium-related disorders. Imaging and tissue analysis are key to assessing gland health.
- The glands’ posterior location requires careful surgical access to avoid thyroid damage.
- Blood vessels’ visibility helps evaluate vascular supply during procedures.
- Chief cell activity is assessed via PTH levels in hyperparathyroidism or hypoparathyroidism.
- Oxyphil cell changes may indicate aging or pathological conditions.
- Micrographs assist in identifying cellular abnormalities or tumors.
The parathyroid glands’ strategic placement and cellular composition underscore their critical role in calcium homeostasis. Their integration with the thyroid’s posterior surface, supported by surrounding cartilages and a robust vascular network, ensures effective hormonal regulation. This detailed understanding enhances clinical approaches to parathyroid-related health concerns.

