Antidiuretic Hormone (ADH), also known as vasopressin, is a crucial hormone with widespread effects on the body, primarily involved in maintaining fluid balance. Produced in the hypothalamus and released by the posterior pituitary gland, ADH plays a vital role in regulating blood pressure, conserving water, and even influencing certain social behaviors. This diagram provides a comprehensive overview of its synthesis, release, and diverse physiological actions.
Understanding Antidiuretic Hormone (ADH)
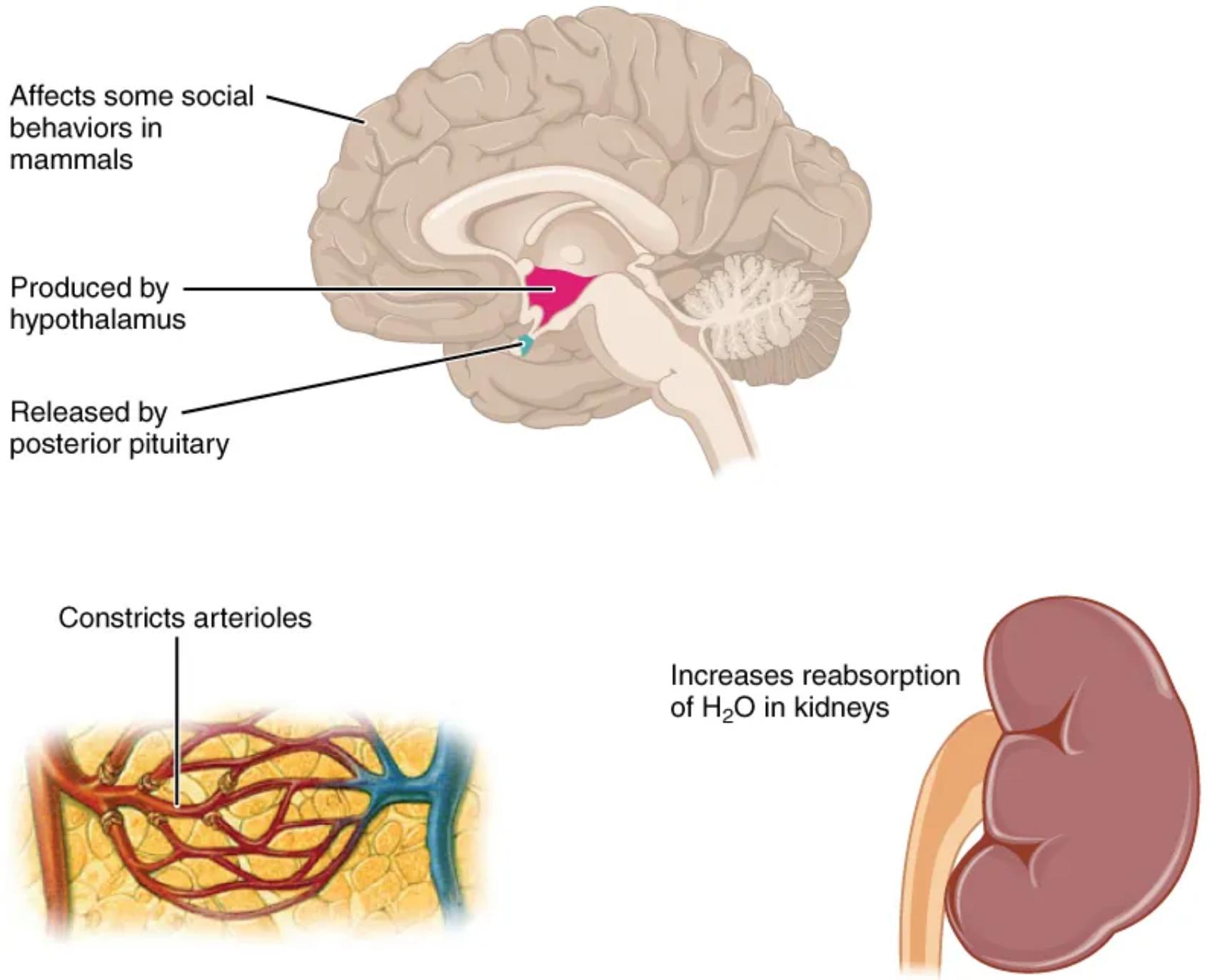
Affects some social behaviors in mammals: Beyond its well-known roles in fluid regulation, ADH has been implicated in influencing various social behaviors in mammals. These behaviors can include pair bonding, maternal care, and aggression, highlighting a complex neurochemical basis for social interactions.
Produced by hypothalamus: The hypothalamus, a vital region of the brain, is responsible for synthesizing ADH. Specialized neurosecretory cells within the hypothalamus produce this hormone, which then travels down axons to the posterior pituitary for storage and release.
Released by posterior pituitary: After synthesis in the hypothalamus, ADH is transported to the posterior pituitary gland, where it is stored. Upon appropriate stimulation, the posterior pituitary releases ADH into the bloodstream, allowing it to exert its effects throughout the body.
Constricts arterioles: One significant action of ADH, particularly at higher concentrations, is to cause the constriction of arterioles. Arterioles are small blood vessels that play a critical role in regulating blood flow and blood pressure. Their constriction leads to an increase in total peripheral resistance and, consequently, an elevation in blood pressure.
Increases reabsorption of H2O in kidneys: This is arguably the most well-known function of ADH. It acts on the renal tubules in the kidneys, increasing their permeability to water. This action promotes the reabsorption of water back into the bloodstream, thereby reducing the volume of urine produced and conserving the body’s fluid content. This mechanism is crucial for maintaining fluid homeostasis.
The Multifaceted Role of Antidiuretic Hormone
Antidiuretic Hormone (ADH), often referred to as vasopressin, is a peptide hormone that is absolutely essential for maintaining the body’s fluid and electrolyte balance. Its primary function is to regulate the amount of water excreted by the kidneys, directly impacting blood volume and blood pressure. The intricate control over ADH synthesis and release underscores the body’s sophisticated mechanisms for maintaining homeostasis.
The journey of ADH begins deep within the brain, specifically in the supraoptic and paraventricular nuclei of the hypothalamus. Here, neurosecretory cells synthesize ADH. Once produced, the hormone doesn’t act immediately; instead, it travels down the axons of these neurons to the posterior pituitary gland, where it is stored in secretory vesicles.
- The posterior pituitary then acts as a release site, secreting ADH into the bloodstream in response to stimuli such as increased plasma osmolality (a higher concentration of solutes in the blood) or decreased blood volume/pressure.
Upon its release, ADH exerts its effects on several target organs. Its most prominent action is on the kidneys, where it significantly increases the reabsorption of water, leading to the production of more concentrated urine and conserving body fluids. Furthermore, at higher concentrations, ADH also acts as a vasoconstrictor, tightening the arterioles and thereby increasing peripheral resistance and blood pressure. Interestingly, research has also illuminated ADH’s role in modulating certain social behaviors, adding another layer of complexity to its physiological significance.
Clinical Significance and Beyond
Dysregulation of ADH can lead to significant health issues. For example, a deficiency in ADH production or release, or a lack of renal response to ADH, results in diabetes insipidus, a condition characterized by excessive urination and intense thirst. Conversely, conditions like the Syndrome of Inappropriate Antidiuretic Hormone Secretion (SIADH) involve excessive ADH release, leading to water retention and hyponatremia (low sodium levels in the blood). Understanding the precise mechanisms of ADH action is therefore crucial for diagnosing and managing these fluid balance disorders. Beyond its clinical implications, the role of ADH in social behaviors opens fascinating avenues for research into the neurobiological underpinnings of social interaction and bonding, showcasing the hormone’s far-reaching influence beyond simple fluid regulation.
The Master Regulator of Water Balance
Antidiuretic Hormone (ADH), also known as arginine vasopressin (AVP), stands as a cornerstone in the body’s elaborate system for maintaining fluid homeostasis. This small yet potent peptide hormone orchestrates several critical physiological processes, primarily focused on regulating water balance and blood pressure. Its synthesis in the hypothalamus and subsequent release from the posterior pituitary gland underscore a powerful neuroendocrine connection that is vital for survival. The body meticulously controls ADH secretion, responding to subtle shifts in plasma osmolality and blood volume, ensuring that water conservation is prioritized when hydration levels are compromised.
The direct effects of ADH are observed across multiple organ systems. In the kidneys, ADH is paramount for concentrating urine; it increases the permeability of the collecting ducts and distal convoluted tubules to water, allowing more water to be reabsorbed back into the circulation rather than being expelled. This mechanism is crucial during states of dehydration, preventing excessive fluid loss and preserving crucial body fluid compartments. Furthermore, ADH acts on the vascular system, inducing the constriction of arterioles. This vasoconstrictive action directly contributes to the maintenance of blood pressure, especially in situations where blood volume might be compromised. Beyond these well-established roles, emerging research highlights ADH’s intriguing influence on various social behaviors in mammals, suggesting its broader involvement in neurological functions related to social recognition, bonding, and even aggression. This multifaceted nature positions ADH not just as a fluid regulator, but as a hormone with diverse and significant physiological impacts.

