The vascular system serves as the intricate highway of life, transporting oxygen and essential nutrients to every cell in the human body. Among the most critical pathways in this network are the carotid arteries, located on either side of the neck. These vessels are the primary conduits providing blood to the brain, the organ with the highest metabolic demand. When these arteries are clear and elastic, the brain functions at its peak, managing everything from basic motor skills to complex cognitive thought. However, a condition known as carotid artery stenosis can compromise this flow, acting as a silent precursor to some of the most devastating neurological events known to medicine. Understanding the progression of this disease is paramount for anyone looking to safeguard their long-term health and neurological integrity.
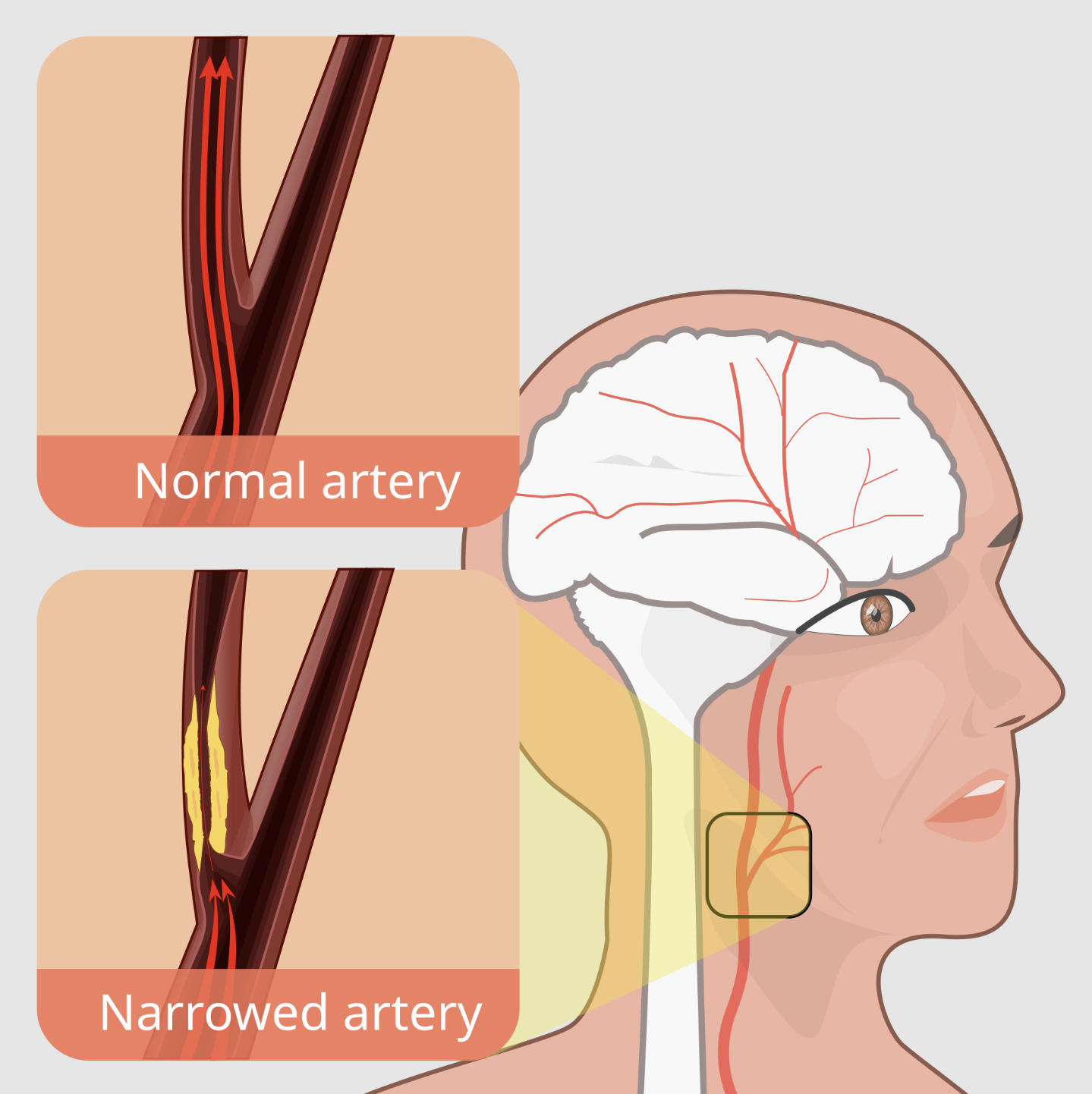
Normal artery: This label identifies a healthy blood vessel characterized by a wide, unobstructed lumen and a smooth endothelial lining. In this state, the carotid artery allows for a high-volume, laminar flow of blood from the heart directly to the brain tissues without resistance.
Narrowed artery: This label illustrates a diseased vessel where significant plaque accumulation has occurred, constricting the internal space available for blood passage. This narrowing, or stenosis, creates turbulent blood flow and significantly increases the risk of complete blockage or the release of emboli into the cerebral circulation.
The Biological Foundations of Carotid Health
To understand the severity of carotid artery stenosis, one must first look at the underlying process of atherosclerosis. This condition involves the gradual buildup of fatty deposits, cholesterol, calcium, and cellular waste products on the inner walls of the arteries. While we often think of this as a simple “clogging of the pipes,” it is actually a complex inflammatory response. The process typically begins with microscopic injuries to the arterial wall, often caused by high blood pressure, tobacco smoke, or elevated glucose levels. These injuries trigger the immune system, leading to the formation of a plaque that progressively thickens and hardens over several decades.
As the plaque grows, the artery loses its natural flexibility. This rigidity further increases the blood pressure within the local area, creating a self-perpetuating cycle of damage. In the carotid arteries, this narrowing is particularly dangerous because of the vessel’s proximity to the brain. Even a partial obstruction can reduce the “reserve capacity” of the brain to handle fluctuations in blood pressure, making the individual more susceptible to injury during periods of physical stress or dehydration. Furthermore, the surface of these plaques can become unstable, rupturing and exposing the underlying tissues to the bloodstream, which triggers immediate clot formation.
Symptoms: Identifying the Silent Warnings
One of the most insidious aspects of carotid artery stenosis is its asymptomatic nature in its early to middle stages. Many individuals may live with a 50% or even 60% blockage without ever feeling a single symptom. The condition is often only discovered during a routine physical exam when a doctor hears a “bruit”—a whooshing sound caused by turbulent blood flow—through a stethoscope. Unfortunately, for many, the first sign of a problem is a medical emergency. When the narrowing becomes critical or a piece of plaque breaks away, it can lead to an ischemic stroke, which occurs when a part of the brain is deprived of oxygenated blood.
Before a full-scale stroke occurs, many patients experience what is known as a Transient Ischemic Attack (TIA). A TIA is essentially a warning stroke that produces temporary symptoms similar to those of a major stroke but resolves within 24 hours. These symptoms may include sudden weakness or numbness on one side of the body, slurred speech, or a temporary loss of vision in one eye, often described as a “shade coming down.” Because these symptoms vanish quickly, many people mistakenly ignore them. However, a TIA is a clear indicator that the carotid artery is significantly compromised and that a major, permanent stroke is likely in the near future without intervention.
Diagnostic Procedures and Imaging Modalities
Modern medicine has developed several non-invasive ways to detect and measure the severity of stenosis. The most common screening tool is the Carotid Ultrasound. This test uses high-frequency sound waves to create images of the arteries and measure the velocity of blood flow. If blood is moving faster than normal through a specific segment, it indicates that the passage has narrowed. This test is highly accurate and involves no radiation, making it an ideal first step for at-risk patients. Clinicians use the results to categorize the stenosis as mild, moderate, or severe, which dictates the subsequent treatment plan.
If the ultrasound results suggest a significant blockage, more detailed imaging might be required. Computed Tomography Angiography (CTA) or Magnetic Resonance Angiography (MRA) can provide three-dimensional views of the vascular anatomy. These tests help surgeons see not only the degree of narrowing but also the composition of the plaque itself. For instance, soft, lipid-rich plaques are generally considered more dangerous than hard, calcified plaques because they are more likely to rupture. In rare or complex cases, a traditional cerebral angiogram may be performed, involving a catheter and contrast dye, to provide the most precise map of the blood vessels possible.
Treatment Paradigms: From Pills to Procedures
The management of carotid artery stenosis depends heavily on the percentage of narrowing and the presence of symptoms. For those with mild to moderate asymptomatic stenosis, the primary goal is medical management. This involves a “statin” medication to lower cholesterol and stabilize the plaque, along with antiplatelet therapy like daily low-dose aspirin to prevent clots from forming. Blood pressure control is also crucial, as it reduces the mechanical stress on the arterial walls. These medications don’t necessarily “clean” the artery, but they significantly lower the risk of the plaque growing or rupturing.
When the stenosis is severe (usually defined as over 70%) or if the patient has had a TIA, surgical intervention is often recommended. The traditional gold standard is a carotid endarterectomy. In this procedure, a vascular surgeon makes an incision in the neck, opens the carotid artery, and physically removes the plaque. It is a highly effective way to restore blood flow and reduce stroke risk. Alternatively, for patients who are at high risk for traditional surgery, carotid artery stenting may be used. This involves threading a catheter through an artery in the groin or arm up to the neck, where a mesh stent is expanded to hold the artery open. Both procedures have excellent success rates when performed by specialized teams.
Long-term Prevention and Lifestyle Synergy
Ultimately, the best way to handle carotid artery stenosis is to prevent it from developing in the first place or to slow its progression through lifestyle choices. Maintaining vascular health requires a proactive approach to diet and exercise. A diet low in saturated fats and high in fiber, fruits, and vegetables can help manage cholesterol levels naturally. Regular aerobic exercise strengthens the cardiovascular system and helps maintain the elasticity of the blood vessels. Perhaps most importantly, the cessation of smoking is the single most impactful change a person can make, as tobacco use is the leading modifiable risk factor for arterial damage.
Beyond diet and exercise, regular monitoring of chronic conditions like diabetes is essential. High blood sugar levels can chemically alter the arterial lining, making it easier for plaques to take hold. By managing these underlying issues and attending regular check-ups, individuals can catch vascular changes before they lead to life-altering complications. Knowledge and prevention are the most powerful tools we have in the fight against carotid disease, ensuring that the vital pipelines to our brains remain clear and functional for a lifetime.

