Hypertension, commonly known as high blood pressure, is frequently referred to by medical professionals as the ‘silent killer.’ This moniker stems from the fact that the condition often progresses for years without presenting any overt symptoms, all while silently inflicting damage upon the body’s most vital organs. When blood travels through the arteries at a pressure that is consistently too high, it creates micro-tears in the vessel walls and forces the heart to work far beyond its intended capacity. Over time, this chronic stress leads to a cascade of physiological failures that can drastically reduce a person’s quality of life or result in fatal outcomes. Understanding how this condition affects various systems is crucial for early intervention and effective management.
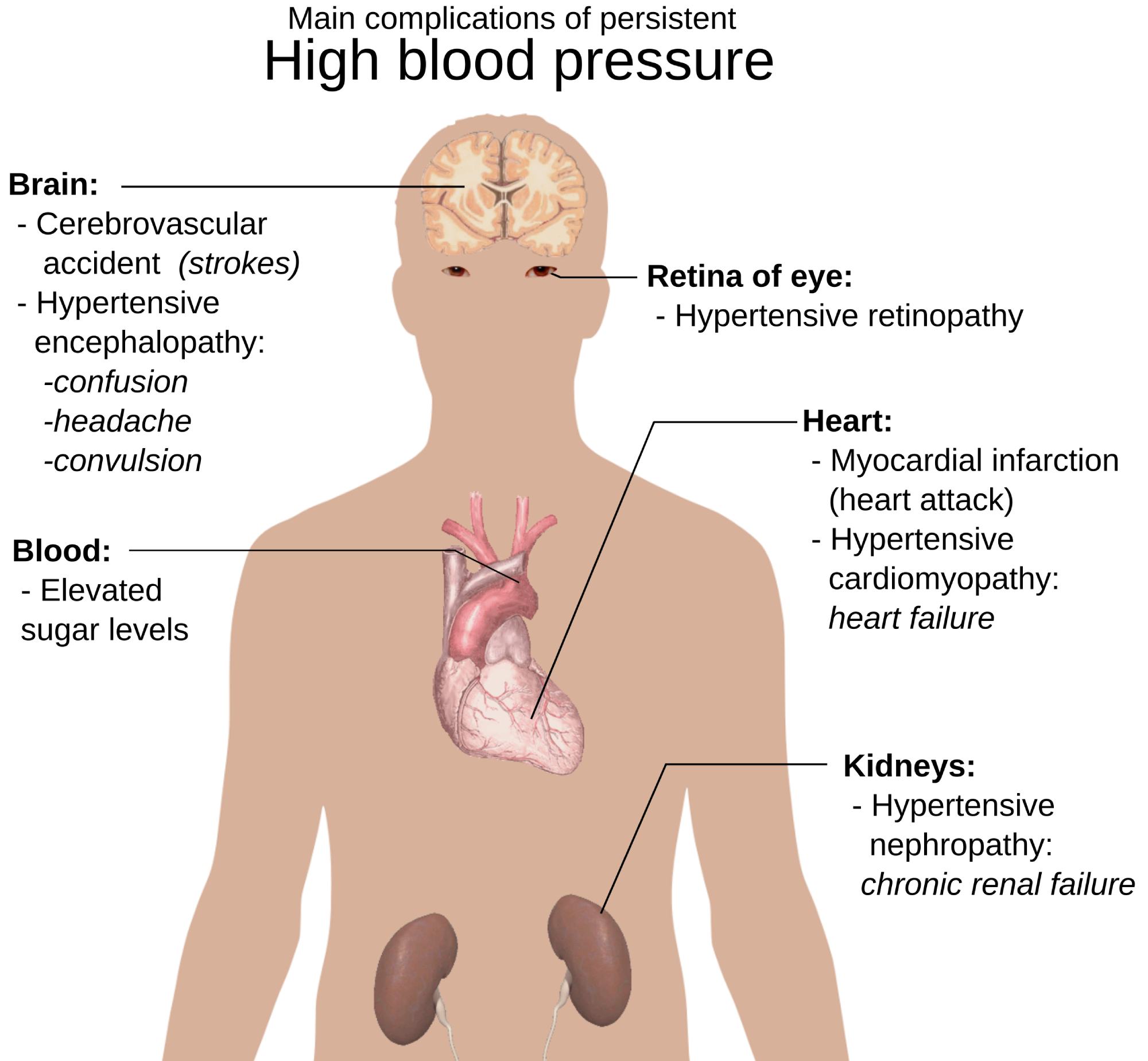
Brain: High blood pressure is the leading risk factor for strokes, as it can cause blood vessels in the brain to either burst or become blocked by clots. It may also lead to hypertensive encephalopathy, a condition characterized by severe confusion, debilitating headaches, and potentially life-threatening convulsions.
Retina of eye: The delicate vasculature within the eyes is highly sensitive to pressure changes, which can lead to a condition known as hypertensive retinopathy. This damage can cause the blood vessels to leak or harden, resulting in blurred vision and, in severe cases, permanent blindness.
Heart: Persistent pressure forces the cardiac muscle to thicken and strain, significantly increasing the likelihood of a myocardial infarction, or heart attack. Furthermore, this chronic workload can lead to hypertensive cardiomyopathy, eventually resulting in the heart’s inability to pump sufficient blood, known as heart failure.
Kidneys: The kidneys function as a sophisticated filtration system that relies on healthy blood vessels; high pressure damages these vessels and leads to hypertensive nephropathy. As the damage progresses, the kidneys lose their ability to filter waste from the blood, which often culminates in chronic renal failure.
Blood: Chronic hypertension is frequently associated with systemic metabolic issues, including elevated sugar levels in the bloodstream. This relationship creates a dangerous synergy that accelerates arterial damage and increases the risk of developing type 2 diabetes and other metabolic disorders.
The Pathophysiology of Arterial Damage
The primary mechanism behind hypertension complications is the mechanical stress placed on the endothelium, which is the inner lining of the blood vessels. When blood flows at a high velocity and pressure, it causes the arterial walls to lose their elasticity and become scarred. This process, known as atherosclerosis, allows plaques of cholesterol and fat to accumulate more easily. As the arteries narrow, the heart must pump even harder to move blood through the restricted passages, creating a self-sustaining cycle of damage that affects the entire cardiovascular events spectrum.
Beyond the structural changes in the vessels, high blood pressure triggers an inflammatory response throughout the body. This end-organ damage occurs because the constant physical trauma to the vessel walls attracts immune cells, which release chemicals that further stiffen the arteries. Over decades, what began as a simple elevation in pressure transforms into a systemic vascular disease that compromises the integrity of every major organ system, from the brain to the distal extremities.
Neurological Risks and Cognitive Decline
The brain is perhaps the most vulnerable organ when it comes to blood pressure fluctuations. While most people fear a massive stroke, hypertension also causes ‘silent’ strokes—small areas of brain tissue death that may not cause immediate symptoms but gradually destroy cognitive function. This cumulative damage is a primary driver of vascular dementia, where patients experience a decline in memory, problem-solving, and reasoning. The brain’s autoregulation system, which keeps blood flow steady, eventually fails under the constant barrage of high pressure, leading to the swelling and neurological deficits seen in encephalopathy.
Furthermore, the high-pressure environment can weaken the walls of cerebral arteries, leading to the formation of aneurysms. If these weakened spots bulge and eventually rupture, they cause a subarachnoid hemorrhage, which is a medical emergency with a high mortality rate. Monitoring blood pressure is therefore not just about heart health; it is a fundamental pillar of preserving long-term cognitive integrity and preventing sudden neurological catastrophes.
Cardiovascular Strain and Structural Remodeling
When the heart is forced to pump against high systemic resistance, it undergoes a process called remodeling. Initially, the walls of the left ventricle thicken to handle the extra load, a condition known as left ventricular hypertrophy. While this helps the heart maintain output in the short term, the thickened muscle eventually becomes stiff and less efficient. This stiffness prevents the heart from filling properly with blood between beats, leading to diastolic heart failure, which can be just as debilitating as the more commonly known systolic failure.
Moreover, the increased oxygen demand of the thickened heart muscle, combined with narrowed coronary arteries, sets the stage for myocardial ischemia. When the demand for oxygen exceeds the supply, the patient may experience angina or a full-scale heart attack. The long-term presence of hypertension also increases the risk of atrial fibrillation, an irregular heart rhythm that can further increase the risk of blood clots and subsequent strokes, illustrating the interconnectedness of these complications.
Renal Integrity and Metabolic Synergy
The relationship between the kidneys and blood pressure is a complex, two-way street. The kidneys help regulate blood pressure by managing fluid balance and secreting hormones like renin. When high blood pressure damages the small filters (nephrons) within the kidneys, they lose their regulatory capacity. This loss causes the body to retain even more salt and water, which in turn drives blood pressure even higher. This feedback loop is why hypertensive patients often see a rapid decline in renal function once the initial damage has been established.
Additionally, as noted in the provided medical illustration, elevated sugar levels often coexist with hypertension. This combination is particularly lethal for the kidneys and the cardiovascular system. High glucose levels further damage the vessel walls and increase oxidative stress, accelerating the progression of nephropathy. Managing both blood sugar and blood pressure is essential, as the presence of one condition significantly worsens the prognosis of the other, leading to a higher incidence of total renal failure and the need for dialysis.
Strategies for Mitigation and Long-term Management
Preventing the severe complications associated with high blood pressure requires a multi-faceted approach involving both medical intervention and lifestyle modifications. Regular screening is the first line of defense, as it allows for the detection of hypertension before significant organ damage has occurred. Once diagnosed, many patients can effectively manage their levels through the DASH (Dietary Approaches to Stop Hypertension) diet, which emphasizes high intake of potassium, calcium, and magnesium while strictly limiting sodium.
Physical activity also plays a critical role, as regular aerobic exercise helps to strengthen the heart and improve the flexibility of the blood vessels. In cases where lifestyle changes alone are insufficient, a wide variety of medications, such as ACE inhibitors, beta-blockers, and diuretics, are available to help bring pressure back to a safe range. By maintaining a proactive stance on vascular health, individuals can significantly lower their risk of stroke, heart failure, and kidney disease, ensuring a healthier and more active future.

