Hypertension, or high blood pressure, is one of the most prevalent yet dangerous medical conditions globally, affecting billions of people. Often described as a silent killer, it typically presents no obvious symptoms while it silently damages the arterial walls and places an immense burden on the cardiac muscle. Because the body can often compensate for elevated pressure for years, many individuals remain unaware of their condition until it manifests as a severe medical emergency. Understanding how hypertension affects the internal anatomy is the first step toward effective prevention and management. By examining the structural changes that occur within the heart and the blood vessels, we can better appreciate the necessity of maintaining optimal blood pressure levels throughout life.
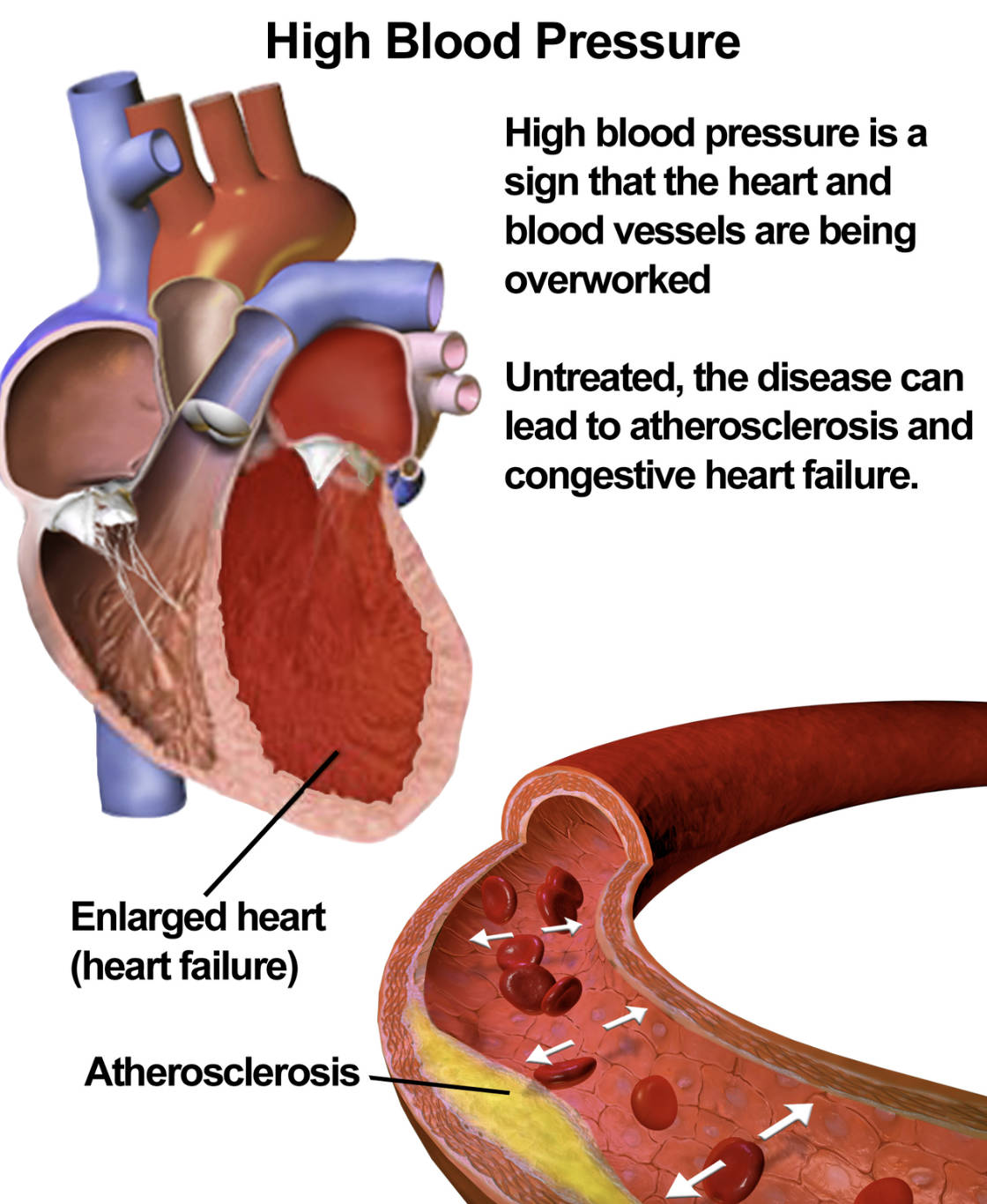
High Blood Pressure: This refers to the clinical measurement of the force exerted by circulating blood against the walls of the body’s arteries. It is the primary hemodynamic stressor that, when chronic, serves as the root cause for various degenerative vascular diseases.
Enlarged heart (heart failure): This condition occurs when the heart muscle thickens and the chambers expand to compensate for the increased workload of pumping against high pressure. Eventually, the heart loses its structural integrity and mechanical efficiency, leading to the clinical syndrome of heart failure.
Atherosclerosis: This pathological process involves the hardening and narrowing of the arteries due to the accumulation of plaque along the endothelial lining. Hypertension accelerates this damage, creating a fertile environment for cholesterol and fatty deposits to restrict essential blood flow to the body.
High blood pressure is a sign that the heart and blood vessels are being overworked: This text highlights the excessive mechanical demand placed on the cardiovascular system when pressures are elevated. Constant overwork leads to cellular changes in the myocardium and the vascular smooth muscle, eventually compromising their functional capacity.
Untreated, the disease can lead to atherosclerosis and congestive heart failure: This warning emphasizes the progressive nature of hypertension if left unmanaged by medical or lifestyle interventions. The transition from simple high pressure to complex systemic failure represents the dangerous trajectory of chronic, uncontrolled cardiovascular strain.
The Physiological Impact of High Blood Pressure
The heart is essentially a muscular pump designed to move oxygenated blood to tissues throughout the body. In the presence of hypertension, the heart must overcome increased systemic vascular resistance to circulate that blood effectively. This extra effort requires the heart muscle, particularly the left ventricle, to grow thicker to generate the necessary force. While this hypertrophy is an initial adaptation, it eventually makes the heart wall stiff and less efficient at filling with blood between beats, reducing the overall cardiac output.
The blood vessels themselves are not passive conduits; they are dynamic structures that respond to mechanical stress. Persistent high pressure causes microscopic tears in the inner lining of the vessels. These lesions initiate a cascade of inflammatory responses, making the vessels less flexible and more prone to damage. Over time, the smooth muscle layer of the artery walls may also thicken, further narrowing the space through which blood can flow and creating a vicious cycle of rising pressure.
Atherosclerosis and Arterial Narrowing
Atherosclerosis is perhaps the most dangerous consequence of uncontrolled hypertension. As plaques—composed of cholesterol, calcium, and cellular waste—accumulate at the sites of vessel damage, the lumen of the artery becomes constricted. This restriction reduces the volume of blood that can reach distal organs, such as the brain, kidneys, and extremities. Chronic hypertension is a primary driver of endothelial dysfunction, which facilitates the rapid progression of these fatty deposits.
The relationship between pressure and plaque is cyclical and destructive. Narrowed arteries further increase blood pressure by forcing the same volume of fluid through a smaller space, which in turn causes more endothelial damage. If a plaque becomes unstable and ruptures, it can lead to the formation of a blood clot. Depending on where this occurs, it can result in a myocardial infarction (heart attack) or an ischemic stroke, both of which are life-threatening events that stem from long-term hypertensive damage.
From Hypertrophy to Heart Failure
When the heart becomes enlarged due to the constant strain of hypertension, it enters a phase of decompensation. An enlarged heart is less flexible and requires significantly more oxygen and energy to function. Over time, the muscle fibers stretch and weaken, leading to a state where the heart can no longer pump enough blood to meet the body’s metabolic demands. This transition into heart failure is often gradual, beginning with mild fatigue and progressing to severe respiratory distress.
Congestive heart failure occurs when the weakened heart allows fluid to back up into the lungs or the extremities. This leads to swelling (edema) and a significant reduction in the patient’s quality of life. The structural changes illustrated in the heart diagram show how the chambers dilate and the walls thin out in the later stages of the disease, representing the final pathway of untreated high blood pressure. Early intervention is the only way to halt this progression before the damage to the myocardium becomes irreversible.
Proactive Management and Prevention
The management of hypertension relies heavily on early detection and consistent lifestyle modifications. Because the condition is often asymptomatic, regular screening through blood pressure checks is essential for adults of all ages. Clinical guidelines often recommend maintaining a blood pressure below 120/80 mmHg to minimize the risk of vascular complications. When lifestyle changes such as reducing sodium intake and increasing aerobic exercise are insufficient, pharmacological intervention becomes necessary.
Modern medicine offers a variety of medications to manage pressure, including diuretics, ACE inhibitors, and beta-blockers. These treatments work by either reducing the volume of fluid in the vessels or relaxing the arterial walls to lower resistance. By taking a proactive approach to heart health—combining a heart-healthy diet like the DASH diet with regular medical check-ups—individuals can successfully manage hypertension and avoid the debilitating consequences of heart failure and atherosclerosis. Prevention remains the most effective tool in the fight against this widespread cardiovascular challenge.

