The human circulatory system is a complex and highly specialized network of vessels designed to transport oxygenated blood and essential nutrients from the heart to every tissue in the body. At the center of this vital transport system are the arteries, which are distinct from veins due to their ability to withstand the high-pressure environment created by the rhythmic pumping of the heart. To manage this mechanical stress, the Artery Wall has evolved into a sophisticated, multi-layered structure that is both resilient and dynamic. Each layer of the arterial wall serves a specific physiological purpose, from providing a smooth surface for blood flow to regulating the diameter of the vessel through muscular contraction. By examining the microscopic anatomy of these vessels, we gain a deeper appreciation for how the body maintains blood pressure and ensures that metabolic demands are met during various levels of physical activity.
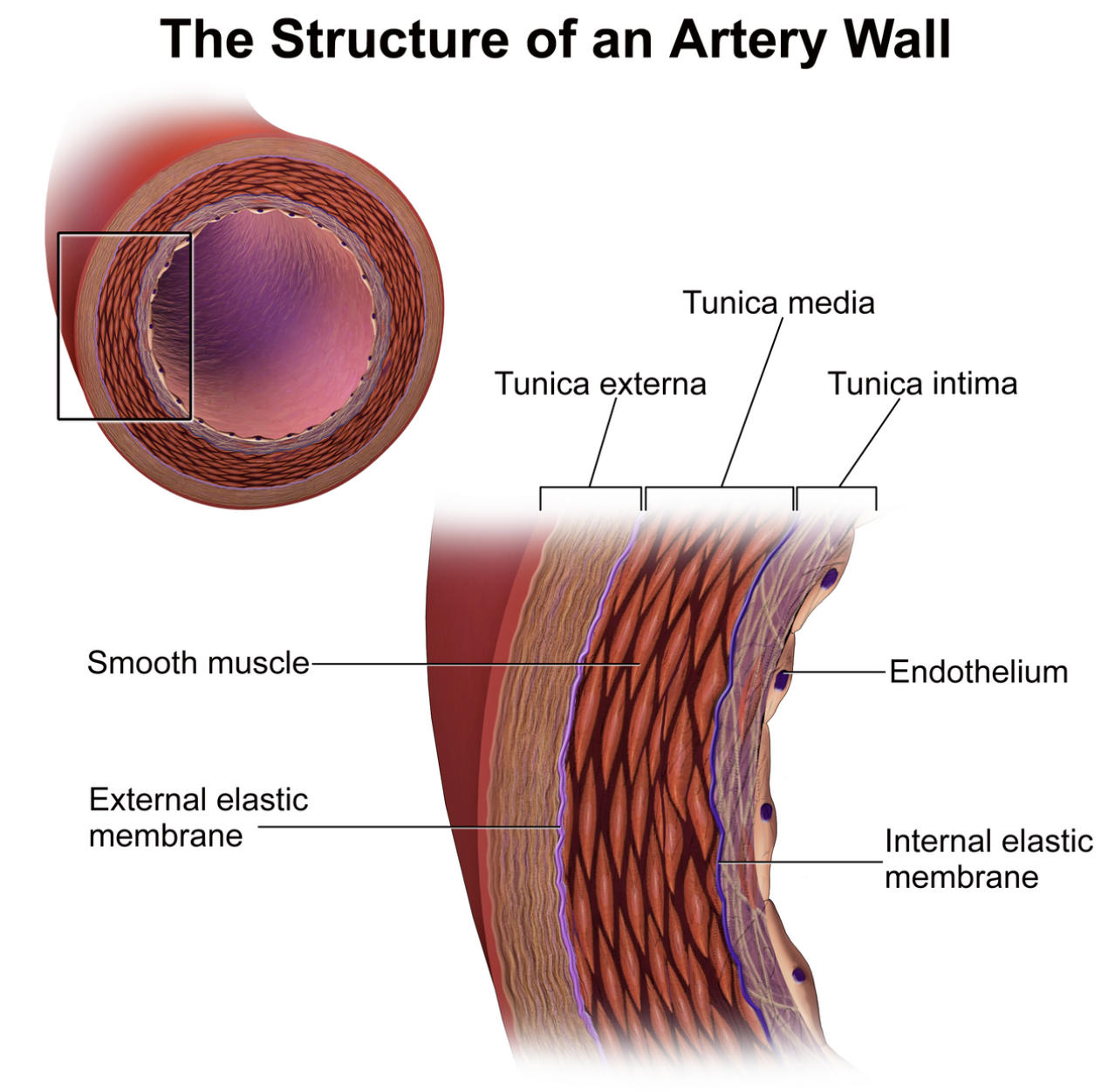
Tunica externa: This is the outermost layer of the artery, composed primarily of collagen and elastic fibers that provide structural integrity and anchor the vessel to surrounding tissues. In larger arteries, this layer also contains small blood vessels known as vasa vasorum that supply the wall itself with nutrients.
Tunica media: This middle layer is typically the thickest part of the arterial wall and consists of smooth muscle cells and varying amounts of elastic tissue. It is responsible for the processes of vasoconstriction and vasodilation, which are critical for controlling blood pressure and flow.
Tunica intima: The innermost layer provides a smooth, frictionless lining for the vessel and is composed of a single layer of squamous epithelium. It acts as a selective barrier and plays a major role in preventing blood clots and regulating vascular tone.
Endothelium: This specialized layer of endothelial cells forms the direct interface between the blood and the vessel wall. It releases signaling molecules like nitric oxide to help the vessel relax and prevents the adhesion of blood cells to the wall.
Subendothelial layer: Positioned just beneath the endothelium, this layer consists of loose connective tissue that supports the overlying cells. It serves as a structural foundation and is one of the first areas affected during the early stages of arterial disease.
Internal elastic lamina: This is a thin sheet of elastic fibers that separates the tunica intima from the tunica media. Its porous nature allows for the diffusion of nutrients from the lumen into the deeper layers of the arterial wall.
External elastic lamina: Located between the tunica media and the tunica externa, this elastic membrane provides additional flexibility to the vessel. It ensures that the artery can stretch under high pressure and return to its original shape without sustaining damage.
Lumen: This is the central hollow space or cavity through which blood circulates throughout the body. The diameter of the lumen is constantly adjusted by the surrounding muscle layers to meet the hemodynamic needs of the organism.
The Tri-Layered Architecture of the Artery Wall
The structural organization of the arterial wall is a marvel of biological engineering, categorized into three primary layers or “tunics.” These layers—the intima, media, and externa—work in unison to ensure that blood is delivered efficiently and safely. While all arteries share this basic tripartite structure, the thickness and composition of these layers can vary significantly depending on whether the vessel is a large elastic artery, like the aorta, or a smaller muscular artery found deeper in the limbs.
The health of the Artery Wall is a primary determinant of overall cardiovascular health. When these layers are flexible and intact, blood flows laminarly, and pressure is kept within a physiological range. However, when the structural integrity of these layers is compromised, it can lead to various systemic issues. The layered design allows for a division of labor: the inner layer handles biochemistry and friction, the middle layer handles mechanical force and movement, and the outer layer handles protection and scaffolding.
Histology and Function of the Tunica Intima
The tunica intima is the most delicate of the three layers, yet it is arguably the most biochemically active. It consists of the endothelium, a basement membrane, and in larger vessels, a subendothelial layer of connective tissue. The endothelium is not merely a passive lining; it is a highly active metabolic organ. It regulates the passage of white blood cells into tissues, influences the formation of blood clots, and produces substances that cause the tunica media to contract or relax.
One of the key features of the tunica intima is the internal elastic lamina. In histological slides, this looks like a wavy line of elastic tissue. This waviness is a result of the vessel being fixed in a constricted state; in a living body under pressure, this lamina stretches to accommodate the pulse of blood. Because it is the layer in direct contact with blood, the tunica intima is particularly susceptible to damage from high cholesterol, toxins from smoking, and high blood glucose levels.
The Muscular Power of the Tunica Media
The tunica media is characterized by its concentric layers of smooth muscle and elastic fibers. This layer is what gives arteries their characteristic thickness and allows them to maintain their shape even when they are not filled with blood. The smooth muscle cells here are regulated by the autonomic nervous system and local chemical signals. When the muscle fibers contract, the lumen narrows (vasoconstriction), increasing blood pressure. When they relax, the lumen widens (vasodilation), decreasing blood pressure and increasing local blood flow.
In elastic arteries, the tunica media contains a high proportion of elastic fibers. This allows vessels like the aorta to act as a “pressure reservoir.” During systole, the heart pumps blood into the aorta, causing it to expand. During diastole, the elastic recoil of the tunica media pushes the blood forward, ensuring a continuous flow even when the heart is between beats. In muscular arteries, the smooth muscle predominates, allowing for fine-tuned control over which organs receive more or less blood at any given time.
Structural Support from the Tunica Externa
The tunica externa, also known as the tunica adventitia, serves as the protective sheath of the artery. It is composed primarily of collagen fibers that blend into the surrounding connective tissue, effectively anchoring the blood vessel in place so it does not shift during movement. This layer is essential for preventing the over-expansion of the artery; without the tough collagenous support of the externa, the internal pressure of the blood could cause the vessel to rupture.
Interestingly, the walls of large arteries are so thick that the inner layers cannot receive enough oxygen or nutrients through simple diffusion from the blood in the lumen. To solve this, the tunica externa contains the vasa vasorum, literally meaning “vessels of the vessels.” These tiny capillaries penetrate the outer layers of the artery to provide the living tissue of the wall with its own dedicated blood supply. Additionally, a network of nerves known as the nervi vasorum resides here to control the smooth muscle in the media.
Pathophysiology: When the Wall Fails
Understanding the anatomy of the artery wall is critical for understanding cardiovascular diseases. The most common pathology is atherosclerosis, a condition where fatty deposits, or plaques, build up in the tunica intima. This process often begins with damage to the endothelium, allowing lipids to enter the subendothelial space. Over time, this leads to chronic inflammation, the migration of smooth muscle cells from the media to the intima, and eventually, the calcification of the vessel wall.
- Aneurysm: A weakening of the arterial wall, usually in the tunica media, that causes a bulge to form. If the pressure becomes too great, the wall can rupture, leading to life-threatening internal bleeding.
- Arterial Stiffness: As we age, the elastic fibers in the tunica media may degrade and be replaced by stiffer collagen. This increases systolic blood pressure and puts more strain on the heart.
- Vasculitis: An autoimmune condition where the body’s immune system attacks the artery wall, causing inflammation and narrowing of the lumen.
- Hypertension: Chronic high blood pressure causes the tunica media to thicken and the lumen to narrow, creating a dangerous cycle of increasing resistance.
Maintaining Vascular Health and Resilience
Preserving the integrity of the Artery Wall is the cornerstone of longevity. Lifestyle choices play a massive role in how these layers age and function. For example, regular aerobic exercise promotes the health of the endothelium by increasing the production of nitric oxide, which keeps the vessels flexible. A diet low in saturated fats and high in antioxidants helps prevent the oxidative stress that triggers plaque formation in the tunica intima.
Furthermore, managing blood pressure is essential to prevent the mechanical fatigue of the elastic laminae. When pressure is consistently high, the constant stretching can lead to micro-tears and permanent structural changes. By understanding the intricate labels and layers of the arterial wall, patients and students alike can better visualize why healthy habits are necessary. The artery is not just a tube; it is a living, breathing, and reacting organ that demands care and protection to keep the entire human machine running smoothly.
In conclusion, the structure of an artery wall is a perfect example of the relationship between form and function in human anatomy. From the microscopic endothelial cells that manage blood chemistry to the robust collagen fibers of the tunica externa that provide strength, every component is vital. Maintaining these structures through proper medical care and lifestyle choices ensures that the circulatory system can continue its tireless work of sustaining life.

