Explore the essential role of the major salivary glands in oral health and digestion with this detailed anatomical guide. Learn about the parotid, submandibular, and sublingual glands, and how their ducts deliver saliva to lubricate, protect, and initiate the breakdown of food in the mouth.
Saliva, often underestimated, is a vital bodily fluid produced by a network of salivary glands, playing a critical role in maintaining oral health and initiating the digestive process. The major salivary glands, strategically located around the oral cavity but outside the oral mucosa, are responsible for secreting the bulk of our daily salivary output. Understanding their anatomy and function is key to appreciating their contribution to digestion, speech, taste, and the prevention of oral diseases.
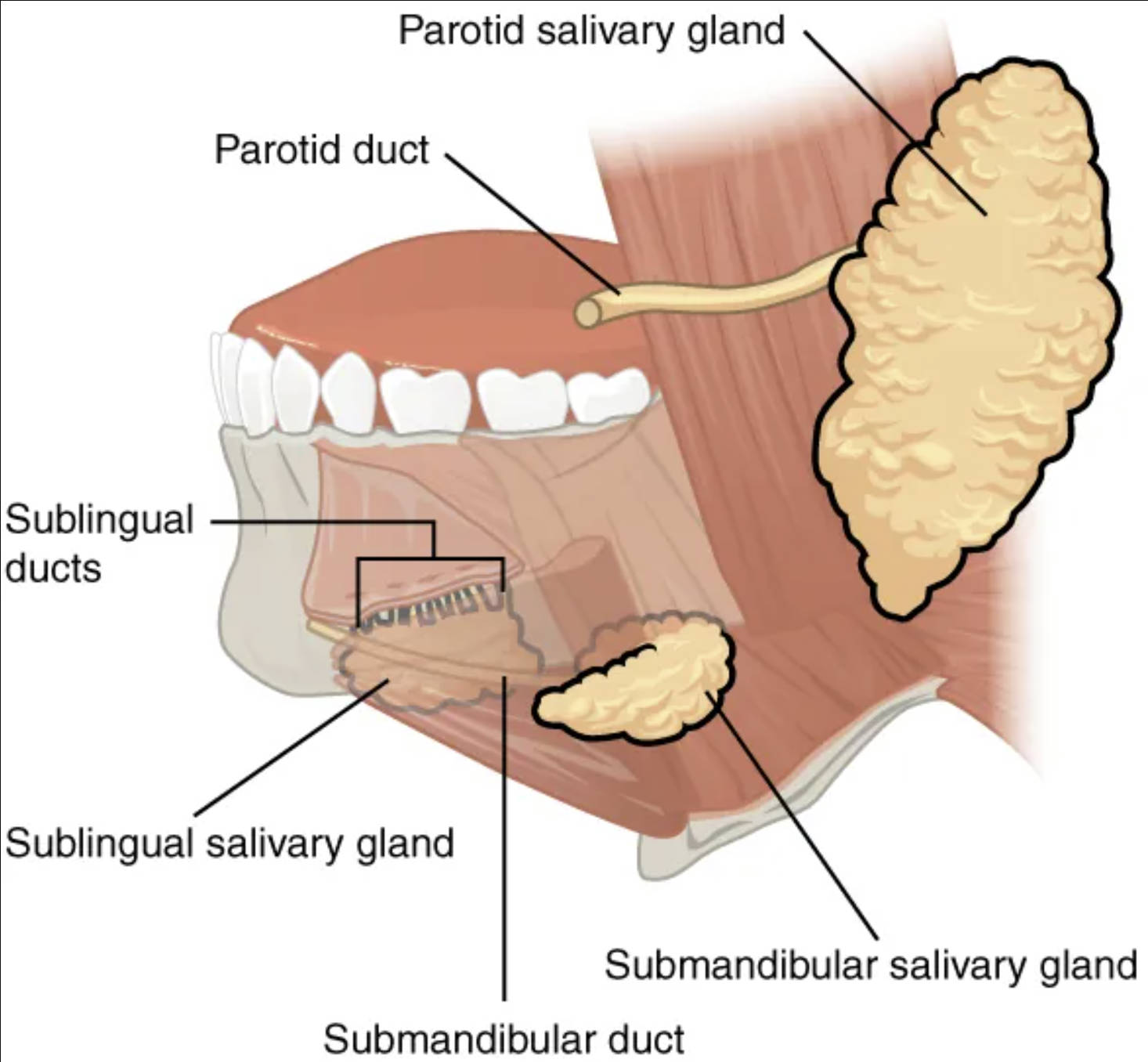
Parotid salivary gland: The parotid gland is the largest of the major salivary glands, located just anterior to the ear. It produces a serous, watery saliva rich in enzymes, particularly salivary amylase, which begins the digestion of carbohydrates.
Parotid duct: Also known as Stensen’s duct, the parotid duct transports saliva from the parotid gland into the oral cavity. It opens into the mouth opposite the second upper molar tooth.
Sublingual ducts: These are several small ducts that emerge from the sublingual salivary gland to empty saliva directly into the floor of the mouth. They contribute to the moistening of the oral cavity.
Sublingual salivary gland: The sublingual gland is the smallest of the major salivary glands, situated beneath the tongue. It produces a predominantly mucous saliva, contributing to lubrication and buffering within the mouth.
Submandibular salivary gland: The submandibular gland is located beneath the floor of the mouth, medial to the body of the mandible. It produces a mixed serous and mucous saliva, making a significant contribution to total saliva volume.
Submandibular duct: Also known as Wharton’s duct, this duct carries saliva from the submandibular gland to the oral cavity. It opens at the base of the lingual frenulum on the floor of the mouth.
The Indispensable Role of Saliva and Salivary Glands
The production and secretion of saliva by the salivary glands are fundamental processes with far-reaching implications for human health. Saliva is not merely water; it is a complex fluid containing enzymes, electrolytes, mucus, and antimicrobial compounds, each playing a crucial role. The major salivary glands—the parotid, submandibular, and sublingual glands—work in concert to ensure a continuous supply of this vital fluid. Their placement outside the oral mucosa, with saliva delivered into the mouth via a system of ducts, exemplifies the efficiency of the human anatomical design.
The critical functions of saliva include:
- Lubrication: Moistening food to aid in chewing and swallowing, and lubricating the oral tissues to facilitate speech.
- Digestion: Initiating carbohydrate digestion with salivary amylase and fat digestion with lingual lipase (though the latter becomes active in the stomach).
- Taste: Dissolving taste-producing molecules so they can interact with taste buds.
- Protection: Washing away food debris, buffering acids to maintain oral pH, and containing antibacterial agents like lysozyme and lactoferrin to protect against pathogens.
- Remineralization: Providing calcium and phosphate ions that help in the repair of tooth enamel.
Each of the major salivary glands contributes uniquely to the composition and volume of saliva. The parotid gland is predominantly serous, producing a watery fluid rich in amylase. The submandibular gland produces a mixed secretion, combining both serous and mucous components, making it a major contributor to total salivary flow. The sublingual gland, being primarily mucous, provides a thicker, more viscous saliva important for lubrication and protection. Disorders affecting these glands, such as sialadenitis (inflammation) or salivary stones (sialolithiasis), can significantly impair salivary production, leading to conditions like xerostomia (dry mouth), which can have detrimental effects on oral health and quality of life. Understanding the intricate workings of these glands is crucial for diagnosing and treating such conditions, reinforcing the importance of maintaining proper salivary gland function for overall well-being.
In summary, the major salivary glands—parotid, submandibular, and sublingual—are indispensable components of our oral and digestive systems. Their anatomical placement and the sophisticated ductal system they employ allow for the efficient delivery of saliva, a fluid critical for everything from the initial breakdown of food to protecting against oral pathogens. Maintaining the health of these glands is vital for preserving oral integrity, facilitating proper digestion, and ensuring overall physiological balance.


I have had dry mouth for the last few years. My dentist prescribed flouride tooth paste and have triied all remedies typically found online. ( Of which I have tries.) He mentioned a prescription medication but reticent to prescribe as he wanted my primary Dr to do. I don’t know how this dry mouth started and why and have no answers of what remedy to use. I really need a remedy for this condition. Is there one?