The human brain is one of the most metabolically active organs in the body, requiring a constant and high-volume supply of oxygenated blood to function correctly. This vital supply is primarily delivered through the carotid arteries, two large blood vessels located on either side of the neck. When these vessels remain clear and flexible, the brain receives the nutrients it needs to maintain cognitive function and motor control. However, when the internal environment of these arteries changes due to the accumulation of fatty deposits, a condition known as carotid artery stenosis develops. This condition is particularly dangerous because it often progresses without any noticeable symptoms until it triggers a significant neurological event, making it a major focus of preventative vascular medicine.
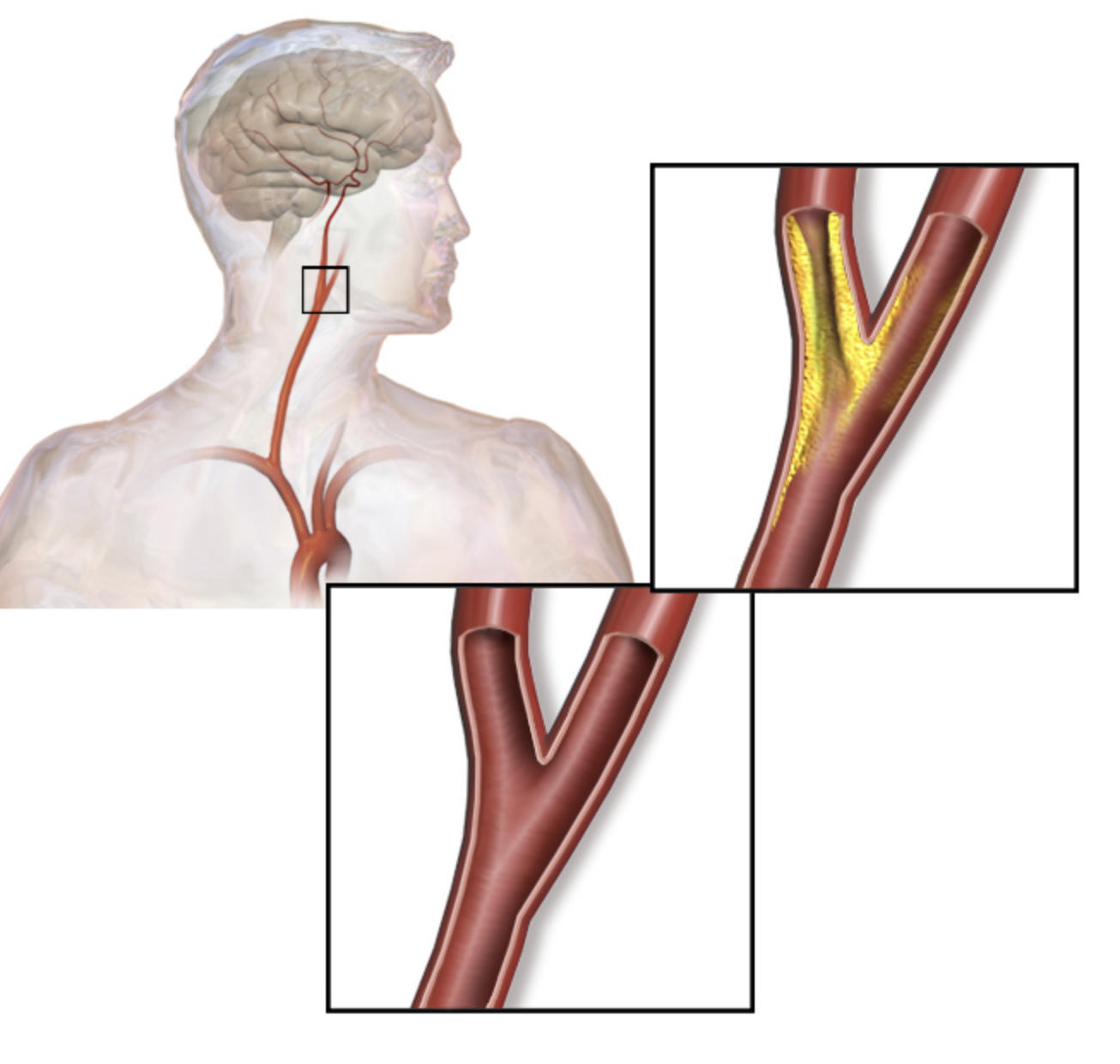
Overview of the Carotid Artery System: This portion of the diagram shows the anatomical path of the carotid arteries as they ascend from the chest into the head. It highlights the critical connection between the heart’s output and the brain’s survival, emphasizing the vulnerability of this pathway to vascular disease.
Healthy Carotid Artery: The inset at the bottom displays a healthy arterial bifurcation where the vessel wall is smooth and the interior space is wide. In this state, blood can flow at high velocities without obstruction, ensuring the brain is perfectly perfused even during physical exertion.
Carotid Artery Stenosis: The top inset illustrates a diseased artery where yellow plaque has built up significantly along the vessel walls. This narrowing, or stenosis, creates turbulence in the blood flow and provides a site where blood clots can easily form or break away, potentially leading to a stroke.
The Pathophysiology of Plaque Accumulation
The development of carotid artery stenosis is a slow, inflammatory process often spanning decades. It begins with microscopic damage to the endothelium, the thin layer of cells lining the interior of the arteries. This damage can be caused by various factors such as high blood pressure, toxins from tobacco smoke, or high levels of circulating cholesterol. Once the lining is compromised, the body attempts to repair it, but in doing so, it allows fats, calcium, and cellular waste products to become trapped within the vessel wall. This buildup is scientifically referred to as atherosclerosis, a systemic condition that can affect any artery in the body but is particularly hazardous when it occurs in the neck.
As the plaque grows, it does more than just narrow the passage; it changes the texture of the arterial wall. Stable plaques may simply reduce the volume of blood passing through, but unstable or “vulnerable” plaques are prone to rupturing. When a plaque ruptures, the body’s clotting mechanism is activated, forming a thrombus on the site. If this clot becomes large enough, it can block the artery entirely, or pieces of the clot and plaque can break off and travel downstream into smaller vessels in the brain, causing an immediate blockage and subsequent tissue death.
Recognizing the Warning Signs: TIAs and Strokes
One of the most challenging aspects of this disease is that it is often asymptomatic until a crisis occurs. However, some patients may experience a transient ischemic attack, which is frequently described as a “mini-stroke.” During a TIA, blood flow to a part of the brain is temporarily restricted, causing symptoms like sudden numbness, difficulty speaking, or loss of vision in one eye. While these symptoms usually resolve within minutes or hours without permanent damage, they are a critical warning sign that a major stroke may be imminent. Ignoring a TIA is a missed opportunity for life-saving medical intervention.
If the blockage is severe or permanent, it results in an ischemic stroke, which can lead to long-term disability or death. The severity of the outcome depends on which part of the brain was deprived of oxygen and for how long. Common symptoms include facial drooping, arm weakness on one side of the body, and slurred speech. Because brain cells begin to die within minutes of losing their blood supply, immediate medical attention is required to attempt to restore flow through clot-busting medications or mechanical procedures.
Risk Factors and Preventive Measures
While some risk factors for stenosis, such as age and family history, are unavoidable, many of the primary drivers are lifestyle-related. Smoking remains one of the most significant contributors, as it both damages the arterial lining and increases the likelihood of blood clots. Chronic conditions like diabetes and hypertension also accelerate the hardening of the arteries. High levels of low-density lipoprotein (LDL) cholesterol are the raw materials for plaque, making dietary management and lipid-lowering therapies essential for those at risk.
Prevention focuses on managing these comorbid conditions. Regular exercise helps maintain arterial elasticity and assists in weight management, which reduces the overall strain on the cardiovascular system. A diet rich in fiber, healthy fats, and antioxidants can help stabilize existing plaques and prevent the formation of new ones. For individuals at high risk, doctors may prescribe low-dose aspirin or other antiplatelet medications to reduce the stickiness of the blood, making it less likely that a clot will form at the site of a narrowed artery.
Diagnostic Tools and Imaging Techniques
Because the disease is silent, screening is vital for individuals with multiple risk factors. The most common first-line diagnostic tool is a carotid ultrasound, a non-invasive procedure that uses sound waves to visualize the arteries and measure the velocity of blood flow. If the blood is moving exceptionally fast through a specific point, it indicates a narrowing. This test provides a percentage of stenosis, which helps clinicians determine the best course of action.
If more detail is needed, doctors may order a CT Angiography (CTA) or Magnetic Resonance Angiography (MRA). These advanced imaging techniques provide a three-dimensional view of the blood vessels and can help distinguish between different types of plaque, such as those that are heavily calcified versus those that are soft and more likely to rupture. In some complex cases, a traditional catheter-based angiogram might be performed, where dye is injected directly into the arteries to provide the clearest possible map of the vascular architecture.
Medical Management and Surgical Intervention
Treatment strategies for carotid artery stenosis are divided into medical management and surgical intervention, depending on the severity of the narrowing and whether the patient has symptoms. For patients with mild to moderate stenosis, the focus is on aggressive risk factor modification and the use of statins to lower cholesterol and stabilize plaque. Monitoring through regular ultrasounds ensures that any progression is caught early before it reaches a critical threshold.
When the narrowing becomes severe (typically over 70%) or the patient has already experienced a TIA, surgical options are considered. The gold standard for many years has been carotid endarterectomy, a procedure where a surgeon opens the artery and physically removes the plaque buildup. Alternatively, carotid artery stenting may be used, especially for patients who are not ideal candidates for open surgery. In this minimally invasive procedure, a mesh tube (stent) is inserted into the artery via a catheter to hold the vessel open and improve blood flow. Both procedures significantly reduce the long-term risk of stroke when performed by experienced vascular teams.

