The image presented demonstrates a classic clinical sign known as pitting edema, a condition characterized by observable swelling in body tissues due to fluid accumulation. This visual guide highlights the standard diagnostic physical examination technique used by healthcare professionals to distinguish this specific type of fluid retention from other forms of swelling. By applying direct pressure to the affected limb, a clinician can assess the severity and nature of the edema based on the tissue’s response.
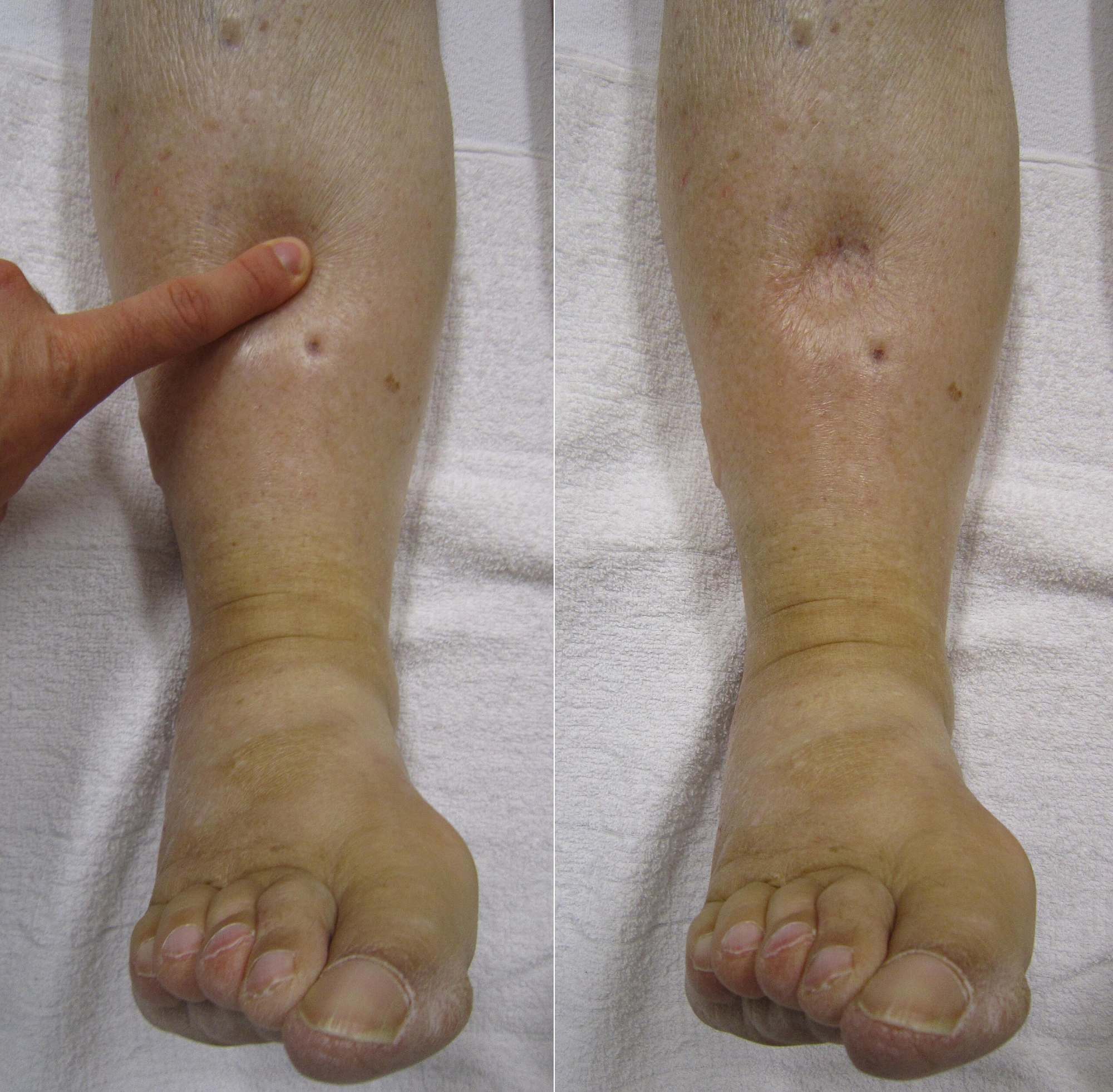
Application of Pressure: The left panel of the image depicts a clinician applying firm, steady pressure with a finger against the patient’s shin, specifically over the pretibial area. This action is performed to displace the excess fluid from the interstitial spaces within the subcutaneous tissue, temporarily pushing it into adjacent areas.
Resulting Indentation: The right panel reveals the immediate aftermath of removing the finger, where a distinct “pit” or depression remains visible on the skin’s surface. This persistent indentation indicates that the fluid has a low protein concentration and moves easily within the tissue, taking several seconds or even minutes to return to the compressed area and fill the void.
Understanding the Mechanics of Fluid Retention
Edema is a palpable swelling caused by an excessive accumulation of fluid in the body’s tissues, most commonly occurring in the feet, ankles, and legs. While swelling can result from injury or inflammation, pitting edema is generally a sign of a systemic issue regarding how the body manages fluid distribution. In a healthy individual, the body maintains a delicate balance of fluids between the blood vessels and the surrounding tissues. When this balance is disrupted, fluid leaks from the capillaries into the surrounding tissue, resulting in the visible swelling seen in the photograph.
The primary mechanism behind this condition involves a disruption in Starling forces, which govern the movement of fluid across capillary membranes. This can occur due to increased hydrostatic pressure (pushing fluid out of vessels) or decreased oncotic pressure (failing to keep fluid inside vessels). For example, if the heart weakens, it cannot pump blood effectively, causing blood to back up in the veins and increasing pressure that forces fluid into the interstitial fluid spaces. Alternatively, a lack of plasma proteins can reduce the holding power of the blood, allowing fluid to escape.
Recognizing the symptoms accompanying the visual sign of edema is crucial for diagnosis. Patients often report that their legs feel heavy or that their shoes feel unusually tight by the end of the day. The skin over the swollen area may appear stretched, shiny, or waxy. While the swelling itself is often painless, the underlying pressure can cause discomfort and limit mobility.
Common characteristics and associated symptoms include:
- A noticeable indentation that remains after pressing on the swollen skin.
- Puffiness or swelling of the tissue directly under the skin, especially in the legs or arms.
- Stretched or shiny skin appearance.
- Increased abdominal size (ascites) in severe cases involving liver disease.
- Difficulty walking due to the heaviness of the limbs.
Pathophysiology and Common Causes
To treat pitting edema effectively, medical professionals must identify the underlying etiology. One of the most prevalent causes is Congestive Heart Failure. In this condition, the heart’s lower chambers lose their ability to pump blood effectively. As a result, blood flow out of the heart slows, and blood returning to the heart through the veins backs up, causing fluid to accumulate in the tissues. This is often gravity-dependent, appearing in the lower extremities of ambulatory patients.
Kidney disease is another significant contributor to this condition. The kidneys are responsible for filtering waste and excess fluid from the body. In conditions like Nephrotic Syndrome, damage to the filtering blood vessels of the kidneys results in declining levels of a protein called albumin in the blood. Albumin acts like a sponge to keep fluid in the blood vessels; when levels drop, fluid leaks into tissues, causing widespread edema. Furthermore, if the kidneys cannot eliminate enough sodium and water, the overall blood volume increases, exacerbating the swelling.
Venous insufficiency is a localized mechanical cause often seen in older adults. The veins in the legs have tiny valves that keep blood flowing up toward the heart. If these valves become damaged or weak, blood can pool in the legs (venous stasis), increasing pressure in the veins and forcing fluid into the surrounding tissue. Unlike systemic organ failure, this cause is often related to the structural integrity of the vascular system in the lower limbs.
Conclusion
Pitting edema is not a disease in itself but rather a significant clinical sign pointing toward an underlying physiological imbalance or medical condition. Whether stemming from cardiac issues, renal dysfunction, or venous insufficiency, the presence of a persistent indentation after pressure warrants a thorough medical evaluation. Understanding the difference between pitting and non-pitting edema aids healthcare providers in narrowing down the differential diagnosis and implementing the appropriate treatment plan, which may range from diuretic therapy to compression stockings or management of the primary organ failure.

