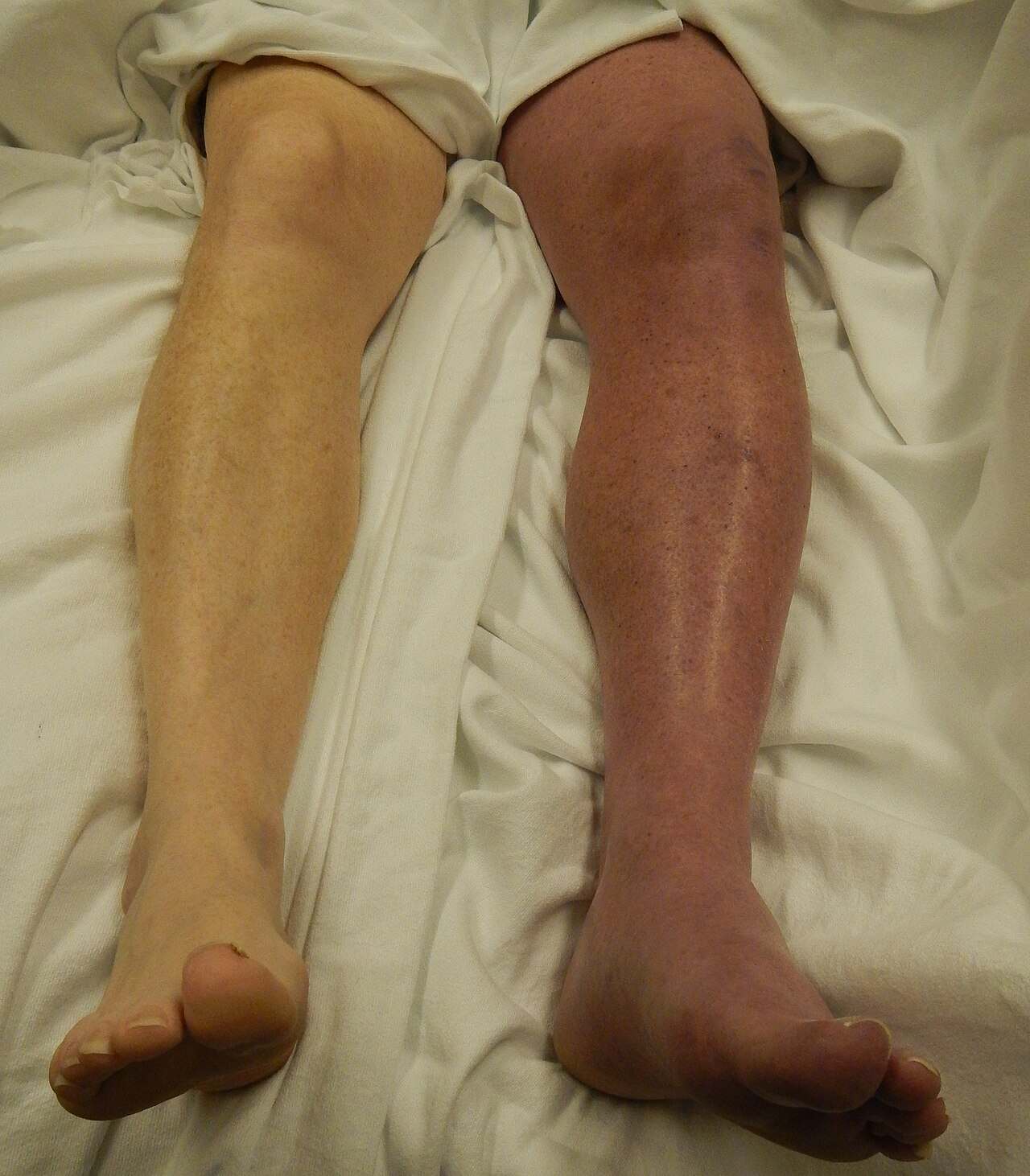
Phlegmasia cerulea dolens is a rare and critical medical emergency resulting from a massive obstruction of the venous drainage system in an extremity, typically the leg. Characterized by profound swelling, severe pain, and a distinct blue or violet discoloration, this condition represents an advanced stage of deep vein thrombosis (DVT) that can rapidly progress to tissue death. The image provided illustrates a striking clinical presentation where the patient’s left leg (appearing on the right side of the image) exhibits the classic signs of venous congestion compared to the healthy, pale appearance of the contralateral limb. Immediate recognition and intervention are vital to prevent venous gangrene and the potential need for amputation.
Clinical Presentation and Significance
Phlegmasia cerulea dolens (PCD), which translates from Latin as “painful blue edema,” is a severe complication of deep vein thrombosis. As seen in the provided image, the affected limb is markedly swollen and discolored. This discoloration, known as cyanosis, occurs because deoxygenated blood is trapped in the tissues due to the near-total blockage of the deep and superficial veins. Unlike a standard DVT, where some collateral blood flow might remain, PCD involves such extensive clotting that venous pressure skyrockets.
The pathophysiology behind this condition involves a dangerous cycle of fluid dynamics. As the veins become blocked, the hydrostatic pressure within the capillaries increases significantly, forcing fluid into the interstitial spaces of the muscle and skin. This massive fluid shift results in the extreme swelling (edema) visible in the photograph. If left untreated, the pressure within the limb can rise so high that it begins to collapse the arteries. This leads to a paradoxical situation: a problem that starts in the veins eventually cuts off the arterial blood supply, depriving the leg of oxygen.
Because of the threat to arterial flow, PCD carries a high risk of morbidity and mortality. It is often associated with underlying hypercoagulable states, such as malignancy (cancer), or severe clotting disorders. The condition is a precursor to venous gangrene, where the tissues begin to die due to ischemia. Therefore, the visual identification of a “blue, swollen leg” is a red flag requiring urgent vascular assessment.
Key clinical features often associated with this condition include:
- Massive Edema: Sudden and severe swelling of the entire extremity.
- Cyanosis: A violaceous (purple) or blue discoloration spreading from the distal foot proximally.
- Severe Pain: Intense, often disproportionate pain caused by tissue ischemia and venous hypertension.
- Coolness to Touch: The limb may feel cold as arterial blood flow is compromised.
- Absence of Pulses: In advanced stages, pedal pulses may be diminished or absent due to compartment pressure.
Pathophysiology of Venous Ischemia
The progression from a common deep vein thrombosis to phlegmasia cerulea dolens is driven by the extent of the thrombotic occlusion. In a typical DVT, a clot obstructs a single vein, but collateral vessels can often bypass the blockage to drain blood from the leg. In PCD, the thrombosis is extensive, often involving the iliofemoral venous segments and their collateral tributaries. This creates a “bottleneck” effect where blood can enter the leg via the arteries but cannot escape through the veins.
As venous pressure exceeds specific thresholds, fluid sequestration into the tissues increases, potentially leading to compartment syndrome. This is a condition where pressure within the muscles builds to dangerous levels, decreasing capillary perfusion pressure. This results in circulatory collapse within the microvasculature of the leg. The tissues suffocate not because blood isn’t being pumped to them, but because the fresh, oxygenated blood cannot enter the high-pressure environment of the leg. This results in significant tissue hypoxia and acidosis.
Etiology and Risk Factors
Identifying the underlying cause is essential for long-term management. PCD is strongly associated with states of extreme hypercoagulability. Malignancy is the most common risk factor; cancers of the lung, pancreas, GI tract, and ovaries are known to release pro-thrombotic factors that can trigger massive clotting. Other risk factors include heparin-induced thrombocytopenia (HIT), antiphospholipid syndrome, and recent major surgeries.
In some cases, the anatomy of the patient contributes to the severity. For instance, May-Thurner syndrome, an anatomical variation where the left common iliac vein is compressed by the right common iliac artery, can predispose individuals to extensive left-leg DVTs. While the image shows the external manifestation, the internal cause is almost always a combination of stasis (lack of blood flow), vessel wall injury, and hypercoagulability—the elements of Virchow’s Triad.
Diagnosis and Therapeutic Management
The diagnosis of PCD is primarily clinical, based on the striking visual appearance of the limb, but is confirmed via Doppler ultrasound or venography. Management is time-sensitive and aggressive. The primary goals are to restore venous outflow, reduce compartment pressure, and prevent the clot from traveling to the lungs (pulmonary embolism).
Treatment strategies often involve systemic anticoagulation with unfractionated heparin to prevent further clot propagation. However, anticoagulation alone is frequently insufficient for PCD. Catheter-directed thrombolysis, where “clot-busting” medication is delivered directly into the thrombus, or mechanical thrombectomy (surgically removing the clot) are often required to rapidly debulk the occlusion. If compartment syndrome is present, a fasciotomy—a surgical procedure to cut the fascia and relieve tension—may be necessary to save the limb from venous gangrene.
Conclusion
Phlegmasia cerulea dolens remains one of the most urgent vascular emergencies encountered in clinical practice. The dramatic visual contrast between the healthy limb and the cyanotic, edematous limb serves as a critical diagnostic clue for healthcare providers. Early recognition allows for the implementation of limb-saving therapies, moving beyond simple anticoagulation to more invasive interventions. By understanding the severe physiological impact of massive venous obstruction, medical teams can effectively mitigate the risks of amputation and systemic complications.

