This article presents a detailed case study of a 2.5-year-old male patient with a known history of asthma, admitted to the emergency department with acute respiratory distress. This case aims to provide medical students and practitioners with insights into the clinical presentation, management, and chest X-ray findings associated with pediatric bronchopneumonia in a complex patient history.
Patient Presentation
A 2.5-year-old male patient, with a known diagnosis of asthma, presented to the emergency department with a 4-day history of cough and shortness of breath, notably without fever. Upon arrival, he exhibited tachypnea, inspiratory and expiratory rhonchi (EU+/+), wheezing, and abdominal breathing.
Initial Management in the Emergency Department
Initial management included two nebulized doses of ipratropium bromide. Despite this, his respiratory clinical condition did not improve. A subsequent dose of ipratropium bromide led to facial flushing (without signs of anaphylaxis or uvular edema).
Following this, a comprehensive treatment regimen was initiated:
- Salbutamol: with proper doses
- Ipratropium Bromide: with proper doses
- Budesonide: with proper doses
- Prednisolone: with proper doses
- Pantoprazole: with proper doses
- Clarithromycin: with proper doses
- Magnesium Sulfate: with proper doses
Laboratory tests revealed a negative acute phase reactant (AFR) but a positive RSV result. During follow-up, as respiratory effort decreased, the doses of magnesium sulfate and salbutamol were reduced. The patient was then admitted to the pediatrics ward for continued monitoring and treatment.
Medical History
The patient is the second twin, born at 34 gestational weeks with a birth weight of 2250 grams. He had an 18-day stay in the Neonatal Intensive Care Unit (NICU). Nine days post-discharge, he was readmitted via ambulance due to respiratory distress. He subsequently had a 4.5-month stay in the Pediatric Intensive Care Unit (PICU), including 3.5 months on intubation. He has a history of recurrent admissions to the ICU, ward, and emergency department.
Family History
There is no known consanguinity between the parents. His twin sibling is healthy.
Physical Examination upon Ward Admission
- General Condition: Moderate
- Oxygen Support: Nasal cannula at 1 L/min
- Skin: Natural, no rash
- Head and Neck: No cervical lymphadenopathy
- Oropharynx: Normal
- Respiratory System: Bilateral rhonchi (+/+), inspiratory and expiratory rhonchi (+/+), no wheezing (-/-), abdominal breathing present.
- Cardiovascular System: S1 and S2 normal, no extra sounds, no murmur, peripheral pulses bilaterally palpable.
- Gastrointestinal System: Abdomen soft, no defense, no rebound tenderness, bowel sounds present, gas and stool passage noted.
- Genitourinary System: Male external genitalia, no hernia, no major urogenital anomalies, urine output present.
- Neuromuscular System: GCS 15, conscious, pupils isochoric, light reflex (+/+), neuromotor development consistent with age, no meningeal irritation signs.
- Extremities: No deformities.
Chest X-ray Findings
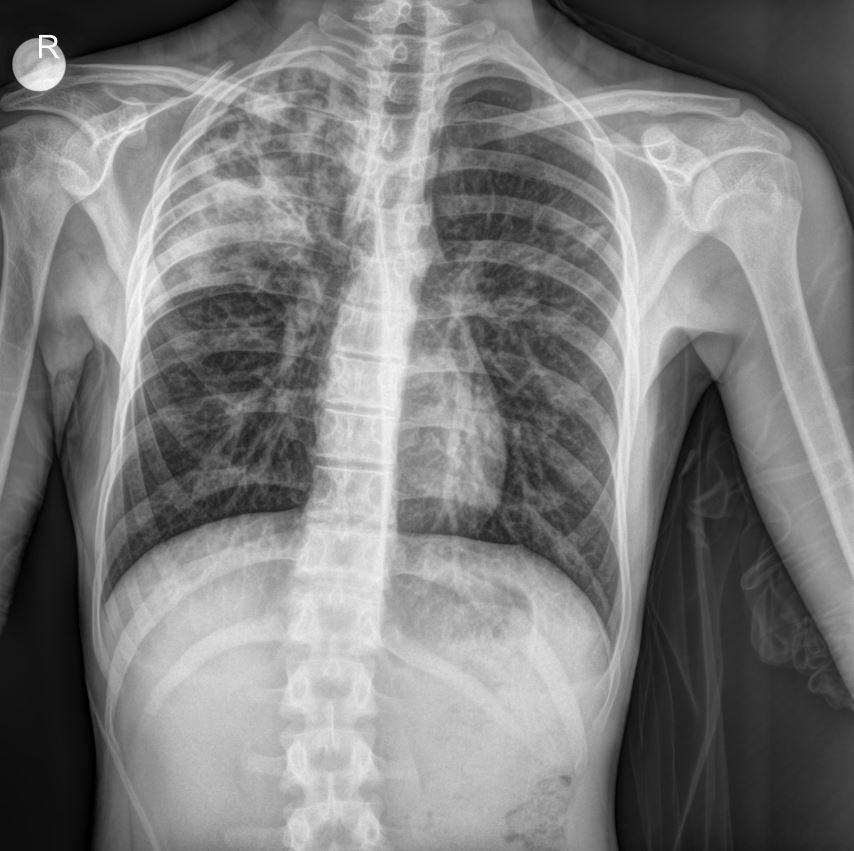
The provided chest X-ray image reveals significant findings consistent with bronchopneumonia, particularly in a patient with a history of recurrent respiratory issues.
- Diffuse Parenchymal Infiltrates: The X-ray demonstrates diffuse, patchy infiltrates predominantly in the right lung field, suggesting areas of consolidation and inflammation. These infiltrates are indicative of bronchopneumonia.
- Bronchial Wall Thickening: There appears to be evidence of bronchial wall thickening, which is commonly seen in patients with asthma and chronic respiratory conditions, exacerbated during acute exacerbations or infections like RSV.
- Hyperinflation: While not overtly severe, some degree of lung hyperinflation may be present, which is also a common finding in asthmatic patients.
- Right-sided Predominance: The infiltrates appear more prominent on the right side, aligning with the clinical presentation of respiratory distress.
These radiological findings, coupled with the positive RSV test and clinical symptoms, strongly support the diagnosis of bronchopneumonia in this young patient.
Current Treatment in the Ward (Day 1 of Admission)
The patient’s general condition is moderate, vital signs are stable, and he is being followed on nasal cannula at 1 L/min.
- Respiratory System: Bilateral rhonchi (++), inspiratory and expiratory rhonchi (++), no wheezing (–), abdominal breathing present.
Medications:
- Salbutamol: with proper doses (4 doses with 2 ml hypertonic saline)
- Ipratropium Bromide: with proper doses
- Budesonide: with proper doses (inhaler)
- Prednisolone: with proper doses (IV) (Day 1)
- Pantoprazole: with proper doses
- Clarithromycin: with proper doses (PO)
- Fortini Multi Fibre 1.5 kcal 200 ML: with proper doses (nutritional supplement)
Home Medication:
- Montelukast Suspension:
Please consult your national drug dosage guidelines or a licensed physician within the relevant department for specific medication types and dosages.
Conclusion
This case highlights the complexities of managing acute respiratory infections like RSV-induced bronchopneumonia in a pediatric patient with a significant history of prematurity, NICU/PICU stays, and pre-existing asthma. The chest X-ray findings visually confirm the presence of parenchymal changes consistent with bronchopneumonia, guiding ongoing management. The multi-faceted approach involving bronchodilators, steroids, antibiotics, and supportive care is crucial in such cases.
Disclaimer: This content is for educational and informational purposes only and should not be considered medical advice or a substitute for professional medical judgment, diagnosis, or treatment.

